Fogarty's Congressional Justification for Fiscal Year 2020 provides justification for activities of the Fogarty International Center, a component of the National Institutes of Health in the U.S. Department of Health and Human Services.
Fogarty is dedicated to advancing the mission of the National Institutes of Health (NIH) by supporting and facilitating global health research conducted by U.S. and international investigators, building partnerships between health research institutions in the U.S. and abroad, and training the next generation of scientists to address global health needs. Learn more about Fogarty's
global health research and research training programs.
To view Adobe PDF files,
download current, free accessible plug-ins from the Adobe's website.
FY 2020 Congressional Justification (Full Text)
Organization Chart
National Institutes of Health
John E. Fogarty International Center
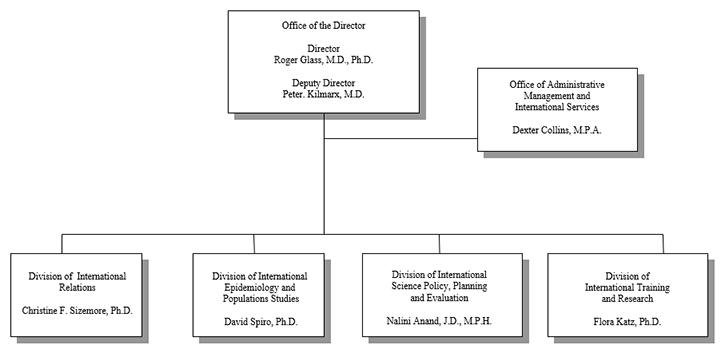
Text Description of Organization Chart
| Office/Division | Name |
|---|
| Office of the Director | Director:
Roger Glass, M.D., Ph.D. |
|---|
Deputy Director:
Peter Kilmarx, M.D. |
Office of Administrative Management and International Services
(to right of Office of Director) | Dexter Collins, M.P.A. |
|---|
Division of International Relations
(below Office of Director) | Christine F. Sizemore, Ph.D. |
|---|
Division of International Epidemiology and Population Studies
(below Office of Director) | David Spiro, Ph.D. |
|---|
Division of International Science Policy, Planning and Evaluation
(below Office of Director) | Nalini Anand, J.D., M.P.H. |
|---|
Division of International Training and Research
(below Office of Director) | Flora Katz, Ph.D. |
|---|
[Top]
Appropriation Language
For carrying out the activities of the John E. Fogarty International Center (described in subpart 2 of part E of title IV of the PHS Act), [$78,109,000] $67,230,000.
[Top]
Amounts Available for Obligation
[Note 1]
(Dollars in Thousands)
| Source of Funding | FY 2018 Final | FY 2019 Enacted | FY 2020 President's Budget |
|---|
| Appropriation | $75,733 | $78,109 | $67,235 |
|---|
| Mandatory Appropriation: (non-add) | | | |
|---|
|
Type 1 Diabetes |
(0) |
(0) |
(0) |
|---|
|
Other Mandatory financing |
(0) |
(0) |
(0) |
|---|
| Rescission | 0 | 0 | 0 |
|---|
| Sequestration | 0 | 0 | 0 |
|---|
| Secretary's Transfer | -178 | 0 | 0 |
|---|
| Subtotal, adjusted appropriation | $75,555 | $78,109 | $67,235 |
|---|
| OAR HIV/AIDS Transfers | 0 | 0 | 0 |
|---|
| Subtotal, adjusted budget authority | $75,555 | $78,109 | $67,235 |
|---|
| Unobligated balance, start of year | 0 | 0 | 0 |
|---|
| Unobligated balance, end of year | 0 | 0 | 0 |
|---|
| Subtotal, adjusted budget authority | $75,555 | $78,109 | $67,235 |
|---|
| Unobligated balance lapsing | -21 | 0 | 0 |
|---|
| Total obligations | $75,534 | $78,109 | $67,235 |
|---|
[Top]
Budget Mechanism - Total
[Note 2]
(Dollars in Thousands)
| Mechanism | FY 2018 Final | FY 2019 Enacted | FY 2020 President's Budget | FY 2020 +/- FY 2019 Enacted |
|---|
| No. | Amount | No. | Amount | No. | Amount | No. | Amount |
|---|
| Research Projects: | Noncompeting | 33 | $7,222 | 48 | $10,480 | 42 | $8,669 | -6 | -$1,811 |
|---|
| Administrative supplements |
(0) | 334 |
(0) | 0 |
(0) | 0 |
(0) | 0 |
|---|
| Competing: | Renewal | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| New | 41 | 7,742 | 29 | 5,425 | 27 | 4,925 | -2 | -500 |
|---|
| Supplements | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Subtotal, competing | 41 | $7,742 | 29 | $5,425 | 27 | $4,925 | -2 | -$500 |
|---|
| Subtotal, RPGs | 74 | $15,297 | 77 | $15,905 | 69 | $13,594 | -8 | -$2,311 |
|---|
| SBIR/STTR | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Research Project Grants | 74 | $15,297 | 77 | $15,905 | 69 | $13,594 | -8 | -$2,311 |
|---|
| Research Centers: | Specialized/comprehensive | 0 | $999 | 0 | $700 | 0 | $643 | 0 | -$57 |
|---|
| Clinical research | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Biotechnology | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Comparative medicine | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Research Centers in Minority Institutions | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Research Centers | 0 | $999 | 0 | $700 | 0 | $643 | 0 | -$57 |
|---|
| Other Research: | Research careers | 53 | $5,534 | 60 | $6,295 | 53 | $5,505 | -7 | -$790 |
|---|
| Cancer education | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Cooperative clinical research | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Biomedical research support | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Minority biomedical research support | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Other | 136 | 32,459 | 137 | 32,726 | 117 | 27,812 | -20 | -4,914 |
|---|
| Other Research | 189 | $37,994 | 197 | $39,022 | 170 | $33,317 | -27 | -$5,705 |
|---|
| Total Research Grants | 263 | $54,290 | 274 | $55,627 | 239 | $47,555 | -35 | -$8,073 |
|---|
| FTTPs | | FTTPs | | | | FTTPs | |
|---|
| Ruth L. Kirschstein Training Awards: | Individual Awards | 0 | $0 | 0 | $0 | 0 | $0 | 0 | $0 |
|---|
| Institutional Awards | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Total Research Training | 0 | $0 | 0 | $0 | 0 | $0 | 0 | $0 |
|---|
| Research and development contracts | 0 | $3,762 | 0 | $3,920 | 0 | $2,975 | 0 | -$945 |
|---|
|
SBIR/STTR (non-add) |
(0) |
(0) |
(0) |
(0) |
(0) |
(0) |
(0) |
(0) |
|---|
| Intramural research | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Res. Management & Support | 58 | 17,503 | 61 | 18,562 | 61 | 16,705 | 0 | -1,856 |
|---|
|
Res. Management & Support (SBIR Admin) (non-add) | (0) |
(0) |
(0) |
(0) |
(0) |
(0) |
(0) |
(0) |
|---|
| Construction | | 0 | | 0 | | 0 | | 0 |
|---|
| Buildings and Facilities | | 0 | | 0 | | 0 | | 0 |
|---|
| Total, FIC |
58 |
$75,555 |
61 |
$78,109 |
61 |
$67,235 |
0 |
-$10,874 |
|---|
[Top]
Major Changes in the Fiscal Year 2020 President's Budget Request
Major changes by budget mechanism and/or budget activity detail are briefly described below. Note that there may be overlap between budget mechanism and activity detail, and these highlights will not sum to the total change for the FY 2020 President’s Budget request for FIC, which is $67.2 million, a decrease of $10.9 million from the FY 2019 Enacted level. The FY 2020 President’s Budget reflects the Administration’s fiscal policy goals for the Federal Government. Within that framework, FIC will pursue its highest research priorities through strategic investments and careful stewardship of appropriated funds.
FIC will support a total of 69 Research Project Grant (RPG) awards in FY 2020, a decrease of 8 awards and $2.3 million, or 14.5 percent, from the FY 2019 Enacted level. Research and training grants decrease by 35 awards and $8.1 million, or 14.5 percent. There is a 24.1 percent decrease in Research and Development (R&D) Contracts and a 10.0 percent decrease in Research Management Support (RMS) which provides in-house research, strategic planning and coordination, as well as administrative and logistical support for FIC and trans-NIH initiatives.
[Top]
Summary of Changes
(Dollars in Thousands)
-
FY 2019 Enacted: $78,109
-
FY 2020 President's Budget: $67,235
-
Net change: -$10,874
| Changes | FY 2020 President's Budget | Change from FY 2019 Enacted |
|---|
| FTEs | Budget Authority | FTEs | Budget Authority |
|---|
| A. Built-in | 1. Intramural research: | | | | |
|---|
| a. Annualization of January 2019 pay increase and benefits | | $0 | | $0 |
| b. January FY 2020 pay increase and benefits | | 0 | | 0 |
| c. Paid days adjustment | | 0 | | 0 |
| d. Differences attributable to change in FTE | | 0 | | 0 |
| e. Payment for centrally furnished services | | 0 | | 0 |
| f. Cost of laboratory supplies, materials, other expenses and non-recurring costs | | 0 | | 0 |
| Subtotal | | | | $0 |
| 2. Research management and support: | | | | |
| a. Annualization of January 2019 pay increase and benefits | | $8,482 | | $12 |
| b. January FY 2020 pay increase and benefits | | 8,482 | | 38 |
| c. Paid days adjustment | | 8,482 | | 32 |
| d. Differences attributable to change in FTE | | 8,482 | | 0 |
| e. Payment for centrally furnished services | | 0 | | 0 |
| f. Cost of laboratory supplies, materials, other expenses and non-recurring costs | | 8,223 | | 0 |
| Subtotal | | | | $82 |
| Subtotal, Built-in | | | | $82 |
| No. | Amount | No. | Amount |
|---|
| B. Program | 1. Research Project Grants: | | | | |
|---|
| a. Noncompeting | 42 | $8,669 | -6 | -$1,811 |
| b. Competing | 27 | 4,925 | -2 | -500 |
| c. SBIR/STTR | 0 | 0 | 0 | 0 |
| Subtotal, RPGs | 69 | $13,594 | -8 | -$2,311 |
| 2. Research centers | 0 | $643 | 0 | -$57 |
| 3. Other research | 170 | 33,317 | -27 | -5,705 |
| 4. Research training | 0 | 0 | 0 | 0 |
| 5. Research and development contracts | 0 | 2,975 | 0 | -945 |
| Subtotal, extramural | | $50,530 | | -$9,018 |
| | FTEs | | FTEs | |
|---|
| 6. Intramural research | 0 | $0 | 0 | $0 |
| 7. Research management and support | 61 | 16,705 | 0 | -1,938 |
| 8. Construction | | 0 | | 0 |
| 9. Buildings and facilities | | 0 | | 0 |
| Subtotal, program | 61 | $67,235 | 0 | -$10,956 |
| Total changes | | | | -$10,874 |
[Top]
Fiscal Year 2020 Budget Graphs
History of Budget Authority: Funding Levels by Fiscal Year
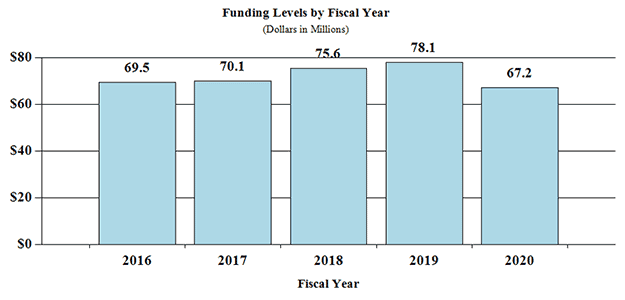
Bar Chart of Funding Levels by Fiscal Year
| Fiscal Year | Funding Level
(Dollars in Millions) |
|---|
| 2016 | $ 69.5 |
|---|
| 2017 | $ 70.1 |
|---|
| 2018 | $ 75.6 |
|---|
| 2019 | $ 78.1 |
|---|
| 2020 | $ 67.2 |
|---|
History of FTEs: FTEs by Fiscal Year
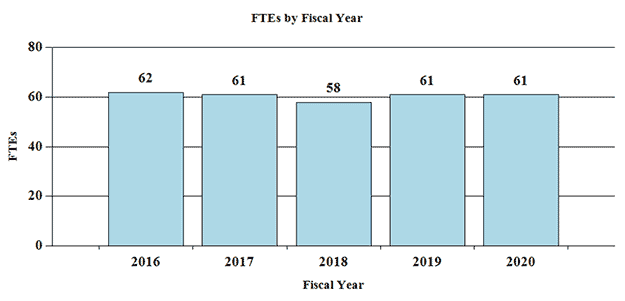
Bar Chart of FTE's by Fiscal Year
| Fiscal Year | FTEs |
|---|
| 2016 | 62 |
|---|
| 2017 | 61 |
|---|
| 2018 | 58 |
|---|
| 2019 | 61 |
|---|
| 2020 | 61 |
|---|
Distribution by Mechanism: FY 2020 Budget Mechanisms
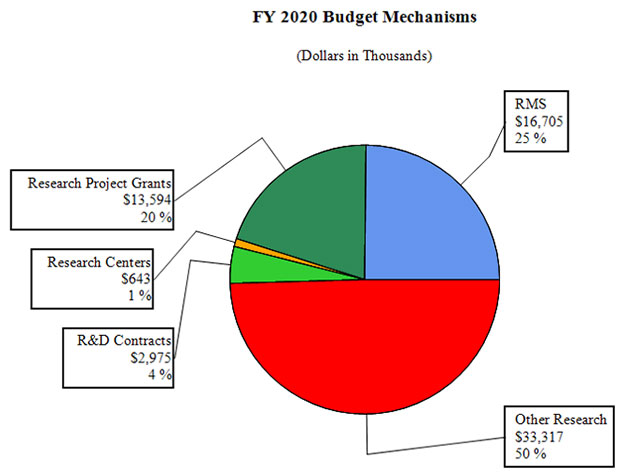
Pie Chart of FY 2020 Budget Mechanisms
| Category | Dollars in Thousands | Percent |
|---|
| R&D Contracts | $ 2,975 | 4% |
|---|
| Research Centers | $ 643 | 1% |
|---|
| Research Project Grants | $ 13,594 | 20% |
|---|
| RMS | $ 16,705 | 25% |
|---|
| Other Research | $ 33,317 | 50% |
|---|
Change by Selected Mechanism: FY 2020 Estimate Percent Change from FY 2019 Mechanism
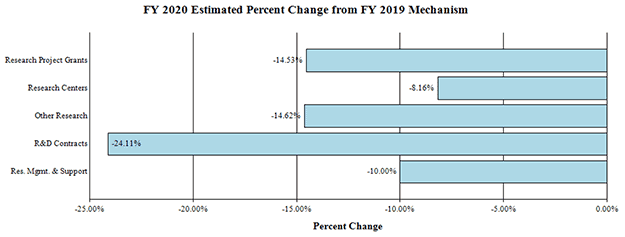
Bar Chart of FY 2020 Estimate Percent Change from FY 2019 Mechanism
| Category | Percent Change |
|---|
| Research Project Grants | -14.53% |
|---|
| Research Centers | -8.16% |
|---|
| Other Research | -14.62% |
|---|
| R&D Contracts | -24.11% |
|---|
| Research Management and Support | -10.00% |
|---|
[Top]
Budget Authority by Activity
[Note 3]
(Dollars in thousands)
| | FY 2018 Final | FY 2019 Enacted | FY 2020 President's Budget | FY 2020 +/- FY 2019 |
|---|
| FTE | Amount | FTE | Amount | FTE | Amount | FTE | Amount |
|---|
Extramural Research
Detail: | Research Capacity Strengthening | | $32,174 | | $33,003 | | $28,005 | | -$4,998 |
|---|
| Development of Human Resources for Global Health Research | | 11,121 | | 11,408 | | 9,680 | | -1,728 |
|---|
| International Collaborative Research | | 14,757 | | 15,137 | | 12,845 | | -2,292 |
|---|
| Subtotal, Extramural |
|
$58,052 |
|
$59,547 |
|
$50,530 |
|
-$9,018 |
|---|
| Intramural research |
0 |
$0 |
0 |
$0 |
0 |
$0 |
0 |
$0 |
|---|
| Research management and support |
58 |
$17,503 |
61 |
$18,562 |
61 |
$16,705 |
0 |
-$1,856 |
|---|
| TOTAL |
58 |
$75,555 |
61 |
$78,109 |
61 |
$67,235 |
0 |
-$10,874 |
|---|
[Top]
Authorizing Legislation
| | PHS Act/Other Citation | U.S. Code Citation | 2019 Amount Authorized | FY 2019 Enacted | 2020 Amount Authorized | FY 2020 President's Budget |
|---|
| Research and Investigation | Section 301 | 42§241 | Indefinite | $78,109,000 | Indefinite | $67,235,000 |
|---|
| International Cooperation | Section 307 | 42§242I | Indefinite | Indefinite |
|---|
| Fogarty International Center | Section 401(a) | 42§281 | Indefinite | Indefinite |
|---|
| Total, Budget Authority | | | | $78,109,000 | | $67,235,000 |
|---|
[Top]
Appropriations History
| Fiscal Year | Budget Estimate to Congress | House Allowance | Senate Allowance | Appropriation |
|---|
| 2011 | $73,027,000 | | $72,914,000 | $70,051,000 |
|---|
| Rescission | $615,089 |
|---|
| 2012 | $71,328,000 | $71,328,000 | $68,653,000 | $69,754,000 |
|---|
| Rescission | $131,835 |
|---|
| 2013 | $69,758,000 | | $69,969,000 | $69,622,165 |
|---|
| Rescission | $139,244 |
|---|
| Sequestration | ($3,494,554) |
|---|
| 2014 | $72,864,000 | | $72,380,000 | $67,577,000 |
|---|
| Rescission | $0 |
|---|
| 2015 | $67,776,000 | | | $67,786,000 |
|---|
| Rescission | $0 |
|---|
| 2016 | $69,505,000 | $68,627,000 | $70,944,000 | $70,447,000 |
|---|
| Rescission | $0 |
|---|
| 2017 [Note 4] | $70,117,000 | $72,141,000 | $73,026,000 | $72,213,000 |
|---|
| Rescission | $0 |
|---|
| 2018 | | $73,353,000 | $74,380,000 | $75,733,000 |
|---|
| Rescission | $0 |
|---|
| 2019 | $70,084,000 | $76,637,000 | $78,150,000 | $78,109,000 |
|---|
| Rescission | $0 |
|---|
| 2020 | $67,235,000 | | | |
|---|
[Top]
Justification of Budget Request
John E. Fogarty International Center for Advanced Study in the Health Sciences
Authorizing Legislation: Section 301 and title IV of the Public Health Service Act, as amended.
Budget Authority (BA):
| BA | $75,555,000 | $78,109,000 | $67,235,000 | -$10,874,000 |
|---|
| FTE | 58 | 61 | 61 | 0 |
|---|
Program funds are allocated as follows: Competitive Grants/Cooperative Agreements; Contracts; Direct Federal/Intramural and Other.
Director's Overview
The Fogarty International Center advances the National Institutes of Health (NIH) mission by supporting and facilitating global health research conducted by U.S. and international investigators, building partnerships between health research institutions in the United States and abroad, and training the next generation of scientists to address global health needs.
Fogarty recently marked its 50th year of advancing science for global health. Fogarty trainees have become scientific leaders and decision-makers and are now training the next generation of researchers in the United States and other countries. Collectively, these efforts have helped build international science networks that are actively tackling emerging infectious diseases and other health problems that affect us all. Fogarty is an integral component of NIH - training scientists for global health research, fostering international research networks, and strengthening the research infrastructure abroad that NIH relies upon to support vital research.
Fogarty’s work benefits America in many ways. For example, training scientists in developing countries equips them to study pandemics at their point of origin, quickly contain outbreaks, and prevent or limit the spread of disease to the United States, thereby ensuring our nation’s safety and security.
Fogarty programs also extend the reach and competitiveness of U.S. universities where there is high demand for international research opportunities. Currently, Fogarty supports over 500 research and training projects involving 100 universities. Roughly 80 percent of Fogarty grants are awarded to U.S. institutions and nearly all Fogarty awards involve U.S. researchers. These U.S. institutions partner with research institutions in low- and middle-income countries (LMICs), helping to build long-term relationships that provide scientific and training opportunities for both partners. Fogarty-facilitated collaboration with international researchers helps these American scientists remain globally competitive and at the forefront of scientific discovery.
Global health research also pays dividends through scientific breakthroughs that result in new treatments that can benefit Americans suffering from the same conditions. Important discoveries in cancer, HIV/AIDS, brain disorders, and child health were based on research conducted in LMICs and are now the basis of treatments in the United States.
Fogarty’s approach is to enable scientists to conduct research where health problems are most prevalent and find solutions with global relevance. In FY 2020, Fogarty will continue to strengthen the scientific workforce in the United States and abroad to conduct research with global impact and address the existing and future threats that affect us all.
Innovations and Discoveries
Strengthening the Biomedical Research Workforce: Since its establishment, Fogarty has supported training for more than 6,000 scientists who represent a diverse and talented biomedical research workforce in the United States and abroad prepared to address emerging and future global health challenges. For example, Fogarty’s Global Health Program for Fellows and Scholars supports U.S. university consortia to provide collaborative, mentored research training in LMICs for researchers from both the United States and LMICs. Recently, Fogarty placed a clinical psychologist who trained at the Morehouse School of Medicine in Atlanta in Liberia, making her the first-ever Fogarty Fellow in the country. She used her fellowship to study the mental health and psycho-social challenges facing communities and individuals affected by the Ebola outbreak. The findings from her fellowship can inform how care is provided following large-scale health emergencies or natural disasters, which is relevant to Liberia as well as disaster-affected communities in the United States.
Investing in the training of global health researchers often has a multiplier effect. For example, in 2011 a Fogarty Fellow and neurologist from Harvard University conducted his fellowship in Zambia, a country that only had three neurologists for a population of more than 14 million. He continued to work in Zambia after his fellowship and recently helped establish Zambia’s first-ever neurology training program to help address this gap.
Past Fogarty trainees are now playing instrumental roles in research funded by other Institutes and Centers at NIH. In 2005, a Peruvian infectious disease specialist received advanced training at the University of Washington through Fogarty’s AIDS International Training and Research Program. The researcher is now a widely-respected infectious disease researcher and was recently selected to lead a trial site in Peru studying the safety and effectiveness of a vaccine for the Zika virus developed by the National Institute of Allergy and Infectious Diseases (NIAID).
Building on Basic Science: Fogarty-supported researchers are translating basic science into clinical knowledge, innovation, and improved health. For example, a novel treatment for hydrocephalus is revolutionizing how the condition is treated and is lowering costs in resource-poor and high-income countries alike. Hydrocephalus is the accumulation of fluid in the brain that is typically treated by the placement of a shunt to drain excess fluid. However, these shunts generally fail within two years, requiring a costly, emergency surgery. Fogarty-supported research in Uganda showed that a novel treatment for hydrocephalus eliminates the need for shunt placement without affecting the neurological development of children. The investigator behind this discovery, a pediatric neurosurgeon from Boston Children’s Hospital, has helped spread the technique, which is now being implemented in major pediatric neurosurgery centers across the United States. The innovative treatment lowers costs and reduces the morbidity and mortality of children who are no longer dependent on shunts for their lifetimes.
In 2006, a Fogarty Fellow in Zimbabwe began work to develop and test a novel, low-cost intervention to address widespread depression. In a country with very few psychiatrists, he trained local grandmothers to deliver talk therapy in public “friendship benches.” His 2012 Fogarty Fellowship at the University of California, Berkeley enabled him to build evidence around the intervention and improve the program. More recently, a randomized control trial funded by Grand Challenges Canada showed that the approach is remarkably effective, and it is now being adapted and deployed in other countries with shortages of mental health professionals. Additionally, community health workers and peer counselors in New York City recently began using the model to help address the high demand for mental health services.
The global effort to combat the HIV epidemic has given millions of people access to antiretroviral therapies, allowing them to live longer with HIV. However, a growing number of people living with HIV (PLHIV) are also acquiring non-communicable diseases (NCDs) as they age. In response to this trend and with support from the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), Fogarty launched “Research to Guide Practice: Enhancing HIV/AIDS Platforms to address NCDs in sub-Saharan Africa”. This effort maximizes the impact of investments the U.S. Government has already made in HIV care in sub-Saharan Africa and builds the evidence base necessary to integrate NCD prevention, care, and treatment into existing HIV care platforms. The project recently developed a research agenda that provides scientists, implementers, and policy makers with a wealth of information which can inform their research questions and investments regarding integrated HIV/NCD care. Another important outcome from this project is the development of mathematical models to predict the burden of NCDs in PLHIV in select countries, which can also inform decision-making at the policy level. Findings from this project can also be utilized to inform NCD care for populations beyond PLHIV both here in the United States and abroad.
Chronic exposure to infectious disease-causing enteric pathogens has a harsh impact on child nutrition and may also lead to cognitive and related developmental deficits. Better understanding of the complex relationships between intestinal pathogens and malnutrition is important to improving the health of children in developing countries as well as in the United States. Fogarty is partnering with the Bill & Melinda Gates Foundation to support an international network of scientists across multiple institutions that recently generated one of the largest, high-quality datasets on the relationship between environmental exposure to pathogens and child development. Findings from this study can inform public health interventions and nutrition strategies for children in the United States and abroad.
Transformational Tools and Technologies: Fogarty-supported researchers have recently made significant advances in developing and harnessing low-cost technologies to improve health. For example, a grantee from Fogarty’s Mobile Health: Technology and Outcomes in Low- and Middle-Income Countries (mHealth) program recently developed and evaluated a smartphone decision support system that assists traditional birth attendants in Guatemala in identifying pregnancy and birth complications during home deliveries. Use of this mHealth tool resulted in more mothers being referred to health care facilities for complications, helping reduce maternal and perinatal mortality.
Fogarty-supported training also enables the development and advancement of innovative tools and technologies. For example, Fogarty-supported research at the University of Virginia led to the development of an inexpensive, anti-bacterial water filter to help prevent childhood diarrheal disease. Recently, a post-doctoral fellow involved in this research project followed it up with additional field tests to improve the filter and recently built a business around it, with current operations in Haiti, Dominican Republic, Mexico, India, Thailand, Uganda, Zambia, and other countries.
Exploring the Next Frontier: Fogarty is preparing for emerging and future threats to global health by building capacity for research and supporting cutting-edge research. Cancer is the second leading cause of death in the world, causing about one in every six deaths. Cancer research in LMICs, where most cancer deaths occur, enables learning that can also improve strategies for the prevention, screening, and treatment of cancer in the United States. Two Fogarty Fellowships and a grant administered by Fogarty and associated with the Medical Education Partnership Initiative (MEPI) helped address this need by building capacity in Malawi for cancer research. MEPI is a partnership between the Office of the U.S. Global AIDS Coordinator, the HIV/AIDS Bureau of the Health Resources and Services Administration, and several NIH Institutes. The grant in Malawi helped catalyze cancer research through improved cancer registries, specialized training, development of a cancer clinic, and establishment of the country’s first pathology lab. Two Fogarty Fellows in Malawi further stimulated the field through their research and networks. Together, these investments laid the groundwork for important publications on HIV-related malignancies and subsequent research grants, as well as the establishment of the Malawi Cancer Consortium, a collaboration between the University of North Carolina at Chapel Hill, the National Cancer Institute (NCI), and several Malawian institutions. The Consortium is now one of the most productive cancer clinical research programs in a low-income country and contributed to recent discoveries in cancer immunotherapy and low-dose chemotherapy.
The rich genetic diversity of African populations likely holds clues to better health for humans across the globe. Until recently, African researchers and African populations had largely been left out of genomics studies, thereby limiting the impact of this field of work. In response to this need, Fogarty, the National Human Genome Research Institute (NHGRI), and the National Institute of Environmental Health Sciences are co-leading the Human Heredity and Health in Africa (H3Africa) program, in collaboration with the NIH Common Fund, eleven other NIH Institutes and Centers, the Alliance for Accelerating Excellence in Science in Africa, and the Wellcome Trust. Recent activities of H3Africa enabled African scientists to develop and use advanced genomics and bioinformatics tools to better understand relationships between genetics, environment, disease, and medicine in Africa. For example, an H3Africa-funded scientist conducted a genomic analysis of the recent Lassa fever outbreak in Nigeria suggesting that rats were responsible for the spread of the disease. The analysis helped Nigerian officials combat the spread of the disease and will help researchers develop a vaccine against it. H3Africa scientists have also made important contributions to genomics research related to high blood pressure, stroke, obesity, and hearing loss.
Priorities
Strengthening the Biomedical Research Workforce: Building on decades of research training experience, the Fogarty International Center will continue to invest in current and future leaders in global health research, strengthening the long-term capacity of research institutions to become sustainable platforms for cutting-edge science, and catalyzing meaningful collaborations between and among institutions in the United States and abroad.
For American researchers, Fogarty offers interdisciplinary and cross-cultural experiences, enabling them to understand the diverse health challenges and opportunities of working in low-resource and international settings and establish partnerships with local researchers to tackle complex global health issues. Fogarty’s Fellows and Scholars program, the Fulbright-Fogarty Fellowship, and the International Research Scientist Development Award offer mentored, research training experiences overseas on health conditions that are not easily studied in the United States. For example, recent Fellows have studied unique health problems such as a rare, pediatric eye cancer in Ethiopia and the connection between skin infection and rheumatic heart disease in Uganda. In FY 2020, Fogarty will continue to provide these types of experiences to enable fellows to become leaders in their fields and contribute to global health research throughout their careers.
Fogarty also supports research training of scientists in LMICs who, with their intimate knowledge of the local context, are uniquely poised to make discoveries with global relevance. Fogarty continues to support training in health areas such as brain disorders, chronic non-communicable diseases, HIV/AIDS, infectious diseases, mHealth, and trauma and injury. Past Fogarty-trained investigators are now leaders in academic institutions and ministries of health in their home countries and are now training the next generation of scientists and leaders in their countries, leading to a compounded return on scientific investment. For example, former Fogarty grantees from the AIDS International Training and Research Program have gone on to develop robust training programs at their home institutions. These Fogarty grantees, along with their own trainees, are making an enormous impact on virtually every area of HIV/AIDS science, including discoveries that have informed treatment protocols now used in the United States. Fogarty will continue to support the training of LMIC scientists as they become global health research leaders in their countries and contribute to science with global relevance.
Looking to the future, Fogarty has recently partnered with the African Academy of Sciences and the Bill & Melinda Gates Foundation to launch the African Postdoctoral Training Initiative (APTI). APTI fellows will train in priority health areas in NIH laboratories and then return to their home countries to become scientific leaders and help train the next generation of investigators in their communities.
Fogarty also prioritizes research and research training for chronic, non-communicable diseases (NCDs), which are becoming increasingly prevalent in LMICs as well as the United States. Alzheimer’s disease, for example, is the sixth leading cause of death in the United States and its prevalence is rising rapidly in LMICs. Fogarty trainees from the United States and abroad are conducting important Alzheimer’s disease research, often through research funded by other NIH Institutes and Centers. For example, Fogarty trainees in Colombia are contributing to the National Institute on Aging’s (NIA) first-ever prevention trial for Alzheimer’s disease in Colombia investigating whether a drug can delay or stop the disease. NIA is also providing supplemental research funding to several Fogarty grantees to expand their research training programs to include Alzheimer’s disease and related dementias. For example, the University of Maryland, Baltimore will work with an institution in Nigeria to improve training on ethics in Alzheimer’s research. Another supplemental award will integrate Alzheimer’s research into an HIV/AIDS research training project in Uganda while a third award will emphasize dementia research in studies with rural populations, also in Uganda. Looking to the future, Fogarty will continue to prioritize research and research training for high-priority NCDs that affect people in LMICs and the United States.
Building on Basic Science: Fogarty is committed to building on basic science research and ensuring that proven health interventions are translated, implemented, and brought to scale. Therefore, Fogarty prioritizes implementation science, which is the study of methods to promote the integration of research findings and evidence into healthcare policy and practice. Implementation science improves the effectiveness and efficiency of the research process and encourages the implementation of policies and programs that are based on robust scientific evidence.
Fogarty continues to support research and research training in implementation science across its extramural programs related to topics such as non-communicable diseases, mental health, trauma and injury, and infectious diseases. For example, Fogarty-supported investigators at Emory University are integrating implementation science into training programs for tuberculosis research (TB) in the countries of Georgia and Ethiopia. Both countries have high burdens of multi-drug resistant TB, which is one of the top ten causes of death worldwide. By integrating implementation science into this program, trainees are better able to produce research findings that will be translated into public health policies and practices.
Building on its investments in implementation science research and training, Fogarty continues to catalyze interactions between researchers, program implementers, and policymakers to maximize public health outcomes and improve the return on investment from U.S. Government programs, such as PEPFAR. An example of this is the Adolescent HIV Prevention and Treatment Implementation Science Alliance (AHISA) - a Fogarty-convened network. AIDS is the leading cause of death of adolescents in Africa, with young women twice as likely to acquire HIV as young men. However, there have been very few studies on treatment and care for this age group, resulting in a poor understanding of how to best implement health services for them. AHISA is a network of NIH-funded scientists conducting relevant implementation research and their in-country partners, including key government representatives, research collaborators, and other stakeholders. Through these collaborations, AHISA enhances the effectiveness of PEPFAR by promoting the use of evidence to improve the prevention, screening, and treatment of HIV among adolescents. Looking to the future, Fogarty will continue to seek out opportunities to leverage implementation science and facilitate greater collaboration between researchers, program implementers, and policymakers to enhance the effectiveness of U.S. Government programs.
Transformational Tools and Technologies: Fogarty continues to stimulate innovation in the development and implementation of low-cost tools, medical devices, and other technologies with the potential to transform global health. For example, Fogarty’s mHealth program supports research to develop or adapt innovative mobile and wireless technologies specifically suited for low- and middle-income countries (LMICs) as well as the study of the effectiveness of interventions delivered through phones and tablets for improving health. An mHealth program grantee from Duke University is currently studying the feasibility, acceptability, and impact of a smartphone app designed to improve adherence to pre-exposure prophylaxis (PrEP) among HIV-positive youth in Thailand. The study is poised to help inform how social media and game-based mechanics can be used to improve adherence to PrEP medications, which may also be relevant for other medications and in other countries, including the United States.
Fogarty recently partnered with the National Institute of Biomedical Imaging and Bioengineering (NIBIB) on a grant to support the launch of a new research center led by Northwestern University focused on the development of low-cost, point-of-care technologies to improve the diagnosis, treatment, and management of HIV/AIDS in rural parts of Africa. The program targets the development and testing of technologies that improve the detection and monitoring of HIV as well as related complications, such as tuberculosis, hepatitis, diabetes, heart disease, and certain cancers. Technologies developed through this program can also be useful for rural areas of the United States, where access to health care facilities and equipment is limited.
Fogarty’s in-house research unit is expanding use of computational modeling, real-time genomic sequencing, and Big Data to better understand disease transmission and outbreak dynamics of threats such as influenza, Ebola, and more. These tools can help improve the effectiveness of vaccines and vaccination strategies and inform the U.S. response to future pandemics.
In FY 2020, Fogarty will continue to harness innovative tools and technologies to advance science with global impact.
Exploring the Next Frontier through Strategic Partnerships: Fogarty serves as a focal point for global health at the NIH, engaging with and supporting other NIH Institutes and Centers by leveraging our investments to advance their research agendas for global health. In addition to robust partnerships across the NIH, Fogarty also works closely with the other Agencies in the U.S. Government. For example, Fogarty partners with the National Science Foundation and the Department of Agriculture on the Ecology and Evolution of Infectious Diseases Initiative, which supports interdisciplinary research on the relationship between environmental factors and the emergence and transmission of infectious diseases.
Beyond the U.S. Government, Fogarty partners with key external public and private entities to further the global health research agenda. For example, Fogarty and other NIH Institutes and Centers collaborate with the South African Medical Research Council to fund U.S. and South African scientists studying HIV/AIDS, tuberculosis and HIV-related comorbidities, and cancers. The partnership harnesses the scientific expertise of both countries, strengthens South African research capacity, and facilitates long-lasting partnerships between U.S. and South African investigators.
Fogarty also leads NIH representation in the Global Alliance for Chronic Diseases (GACD) - a group of 13 international research funders, such as the UK Medical Research Council, the Canadian Institutes of Health Research and the Indian Council of Medical Research. GACD supports research projects that address the prevention and treatment of chronic diseases in vulnerable populations around the world. By engaging a diverse group of funding organizations, GACD is better able to facilitate sharing of best practices, develop international collaborations, and promote complementarity in global health research funding.
In FY 2020, Fogarty will continue to leverage complementary interests and strengths of its partners to advance global health research.
Overall Budget Policy: The FY 2020 President’s Budget request is $67.2 million, a decrease of $10.9 million or 13.9 percent from the FY 2019 Enacted level. Fogarty will continue to advance its mission to support and facilitate global health research, build partnerships between health research institutions in the United States and abroad, and train the next generation of scientists to address global health needs within available funding levels.
Program Descriptions and Accomplishments
Research Capacity Strengthening: The development of effective measures to address shared health challenges requires a critical mass of U.S. and LMIC institutions that can conduct robust research and train the next generation of scientists to solve complex problems. Strong institutions that can conduct health research and train scientists in a wide range of disciplines are critical to finding solutions and to building the research workforce of the future. These institutions can stimulate innovative and multidisciplinary research, generate effective and implementable solutions, and build a nimble and networked research workforce.
Budget Policy: The FY 2020 President’s Budget estimate is $28.0 million, a decrease of $5.0 million, or 15.1% percent, from the FY 2019 Enacted level. Fogarty’s Strategic Plan provides the pathway toward developing sustainable global health research and training programs where they are needed most. Goals of the plan include investing in the critical infectious diseases agenda, as well as mobilizing the scientific community to address the growing epidemic of chronic, non-communicable diseases related to increased longevity and changing lifestyles in the developing world.
Program Portrait: Global Infectious Disease Research Training Program
FY 2019 Level: $6.3 million
FY 2020 Level: $5.4 million
Change: -$0.9 million
As demonstrated by the Ebola outbreak in 2014 and the Zika virus epidemic in 2015, deadly and debilitating emerging infectious diseases can spread rapidly across national borders and continents. Communicable diseases such as malaria and tuberculosis (TB) continue to affect millions of people worldwide. TB is among the top ten causes of death globally, claiming 1.6 million lives annually. Multidrug-resistant TB remains a health security threat as more than half a million new cases in 2017 were resistant to the most effective first-line drug. Additionally, neglected tropical diseases, such as Chagas, trachoma and dengue fever, affect over one billion people globally and cost developing economies billions of dollars every year. Particularly in endemic countries, this unfinished infectious disease agenda requires a robust research workforce that can study transmission patterns, environmental factors, and prevention strategies, while also developing new interventions and tools for diagnosis and treatment.
In 2003, Fogarty launched the Global Infectious Disease Research Training Program (GID) to build critical research capacity among infectious disease scientists across the world. Through a variety of degree programs, short- and medium-term trainings, mentoring, and workshops, U.S. and LMIC institutions work together to address the unique public health and research needs in specific LMIC contexts, preparing researchers to conduct independent infectious disease research in their home institutions. LMIC trainees are paired with U.S. scientists to study a wide range of topics such as tuberculosis, malaria, human papilloma virus, zoonotic foodborne and waterborne pathogens, and many other infectious diseases and related health issues that are endemic to LMICs or impact people living in LMICs. Since its establishment, the GID program has supported the training of over 1,200 researchers, creating a ripple effect as former trainees move into leadership positions and harness their skills to mentor the next generation of infectious disease scientists.
For several years, GID program grantees have conducted research in Mexico to address insecticide resistance related to the prevention and control of dengue fever, an infectious disease transmitted by mosquitoes. The trainees discovered that over time the Aedes aegypti mosquito had developed mutations in their genes causing a strong resistance to the insecticide the Mexican Government used to fight them. Because the Aedes aegypti mosquito is also the main vector for the Zika virus that spread in Brazil and parts of the southeastern United States in 2016, the insecticide spraying campaigns employed to address Zika were less effective than scientists hoped. Applying knowledge of insecticide resistance from their dengue fever research in Mexico, the Fogarty grantees shifted their work to fight the transmission of the Zika virus. Their targeted research produced a simple solution: rotate insecticides every few years to prevent mosquitoes from developing complete resistance, making them more susceptible to the intervention. These findings informed the global response to the Zika outbreak, helping authorities in the United States and abroad maintain the effectiveness of insecticides essential to preventing the spread of the disease.
Sustainable Development of Human Resources for Global Health Research: Breakthrough scientific advances in global health are built upon a foundation of well-trained researchers, over 6,000 to date, from both the U.S. and LMICs, who collaborate to solve major global health problems. Investing in the best and brightest minds, and catalyzing research and training partnerships between talented U.S. and LMIC scientists, continues to be a high priority. Well-trained LMIC researchers bring an understanding of the unique biological, epidemiological, social, and cultural contexts of their communities, thereby contributing this knowledge to research on health challenges that often have broader, global implications.
Budget Policy: The FY 2020 President’s Budget estimate is $9.7 million, a decrease of $1.7 million, or 15.1 percent, from the FY 2019 Enacted level. FIC’s impact has historically been most significant in developing the pipeline of U.S. and foreign research talent. FIC intends to continue support of overseas research experiences available for young U.S. scientists in order to encourage them to adopt careers in global health. FIC will also continue its research training partnerships between U.S. and foreign institutions and strive to enhance research opportunities for foreign scientists when they return to their home countries.
International Collaborative Research: Fogarty-supported research collaborations between U.S. and LMIC scientists make U.S. academic institutions more globally competitive, extend their reach, and enable U.S. scientists to lead and participate in international research teams that address key global health priorities. These partnerships also lead to more robust solutions to global health problems, as the respective strengths and expertise of local and U.S. scientists are brought to bear on complex challenges. Whether the focus is international collaborative research on disorders and diseases of the brain and nervous system, or the prediction and containment of emerging infectious diseases, discoveries and evidence generated by these projects have implications for U.S. populations.
Budget Policy: The FY 2020 President’s Budget estimate is $12.8 million, a decrease of $2.3 million, or 15.1 percent, from the FY 2019 Enacted level. This area supports implementation science to address the “know-do” gap, and would continue research training opportunities for U.S. and foreign scientists, foster a sustainable research environment in LMICs, and build strategic partnerships to further global health.
Program Portrait: Global Noncommunicable Diseases and Injury across the Lifespan
FY 2019 Level: $4.4 million
FY 2020 Level: $3.7 million
Change: -$0.7 million
According to the World Health Organization, in 2016, 71 percent of global deaths were due to chronic, noncommunicable diseases (NCDs), mainly cardiovascular diseases, cancers, diabetes, and chronic lung diseases. Though this burden is shared by all nations, low- and middle-income countries (LMICs) have been disproportionately impacted by NCDs. More than three quarters of NCD deaths (31.5 million) occur in LMICs and the prevalence of NCDs in LMICs is predicted to rise sharply in the coming decades. LMICs additionally bear a greater proportion of the burden of the world’s injuries, one of the leading global causes of death and disability. Injuries can be the result of traffic or industrial accidents, burns, falls, poisonings, pollution, and violence, among other causes.
In an effort to address these high burden health issues, Fogarty has supported international collaborative research and training in NCDs since 2001. Fogarty’s portfolio of NCD-related research and training programs has evolved over time in response to shifting gaps in research and opportunities identified through its research programs. Fogarty’s current flagship research activity is the Global Noncommunicable Diseases and Injury across the Lifespan: Exploratory Research program, which includes small, exploratory research grants for innovative and collaborative biomedical, behavioral, and social science research in the areas of NCDs and injury throughout life in LMICs. The program encourages grantees to engage in diverse scientific approaches including basic, clinical, translational, implementation, and interdisciplinary research to address the wide range of health issues that stem from, or are associated with, different NCDs and injuries. Through this program and others before it, Fogarty has invested in researchers who produce evidence that is critical to understanding the burden, causes, prevention, treatment, and long-term care of NCDs and injuries.
For example, in a collaboration between scientists at the University of Hawaii at Manoa and the Federal University of Rio Grande do Norte in Brazil, program grantees sought to understand how and why adolescent childbirth is associated with chronic conditions and mobility loss as mothers age. Their research on participants from Canada, Albania, Colombia, and Brazil found that women who have their first child before the age of twenty scored higher on the Framingham Risk Score, a tool used to estimate a patient’s future cardiovascular risk. This demonstrates that teenage first-time mothers are at greater risk for heart and blood vessel diseases later in life than are older mothers. These findings can encourage clinicians to be more cognizant of women’s reproductive health when examining their cardiovascular health. The study also provides evidence that clinicians can use to prompt young mothers to be more aware of the other factors that increase their risk for cardiovascular disease, such as unhealthy body weight and physical inactivity. These findings can inform the preventative healthcare of women both in LMICs and in the United States, helping to reduce the global burden of this key NCD.
Research Management and Support (RMS): RMS provides administrative, budgetary, logistical, and scientific support to review, award, and monitor research grants, training awards, and contracts. It encompasses strategic planning, coordination, and evaluation of FIC’s programs; regulatory compliance; international coordination; international science policy; and liaisons with other Federal agencies, Congress, and the public. Specific functions include an in-house epidemiology program performing mathematical modeling of infectious diseases; international program officers developing partnerships between U.S. scientists and institutions and their counterparts abroad to advance scientific research and training; identification of collaborative opportunities with foreign science funding agencies; support for all NIH international travel by issuing and tracking official government passports and international visas; review and approval of Notice of Foreign Travel requests; and the creation and coordination of office travel cables to U.S. Embassies.
Budget Policy: The FY 2020 President’s Budget estimate is $16.7 million, a decrease of $1.9 million, or 10.0 percent, from the FY 2019 Enacted level.
Program Portrait: Influenza Research
FY 2019 Level: $0.5 million
FY 2020 Level: $0.5 million
Change: $0.0 million
This year marked the 100-year anniversary of the 1918 Spanish Influenza pandemic, an unprecedented global crisis during which an estimated 500 million people (one-third of the world’s population) were infected with the virus, resulting in approximately 50 million deaths. A future influenza pandemic would have a severe impact on health in the U.S. and abroad, as well as on the global economy, reducing worldwide GDP by an estimated 5-12 percent. An international outbreak of this scale manifests when the influenza virus spreads from animal reservoirs to humans. Without prior exposure to the virus strain, most humans lack immunity and would thus be at risk for infection. Research on how influenza viruses evolve in animal reservoirs such as birds and swine and how they can infect humans is therefore crucial to avert a future pandemic. Fogarty’s in-house research unit - the Division of International Epidemiology and Population Studies (DIEPS) - works collaboratively with human and veterinary health researchers across the world to study the fundamental dynamics of influenza pandemics including who can be infected, how the virus spreads between locations, and how novel influenza strains are transmitted from animals to humans.
DIEPS researchers utilize several cutting-edge tools, technologies, and techniques to study influenza. They harness Big Data to devise novel influenza surveillance strategies that improve the monitoring of recurrent infections in the U.S. and accelerate the response to an outbreak. For example, they traced the origins of swine influenza viruses that infected over 300 children attending agricultural fairs in the U.S. since 2011 and produced recommendations to limit the spread of zoonotic influenza. Such work helps predict which viral strains will emerge, thereby improving the effectiveness of vaccines. DIEPS is additionally at the forefront of novel research that connects genomic analysis with epidemiological computational modeling to study how new animal influenza viruses evolve and the effects of population dynamics and trade flow on the generation of such viral strains. Computational modeling allows researchers to understand factors that affect the spread of influenza, such as population structures, spatial diffusion, and climatic conditions. Utilizing novel data streams such as anonymized mobile phone and insurance records, high resolution climate data, internet queries, and social media mentions provide epidemiological information that can be vital in the event of outbreak. DIEPS scientists also analyzed historical records of mortality and morbidity from previous influenza pandemics to inform the response to future pandemics, a discipline they are pioneering as “archaeo-epidemiology.” They have tracked the evolution of influenza viruses in swine, birds, and canines globally, allowing them to predict future pandemics and protect agriculture from threats.
These important influenza research efforts help ensure that the U.S. Government has the best science available to respond appropriately and rapidly to a future influenza pandemic.
[Top]
Budget Authority by Object Class
[Note 5]
(Dollars in thousands)
| | FY 2019 Enacted | FY 2020 President's Budget | FY 2020 +/- FY 2019 |
|---|
| Total compensable workyears: | | | |
|---|
| | Full-time employment | 61 | 61 | 0 |
|---|
| | Full-time equivalent of overtime and holiday hours | 0 | 0 | 0 |
|---|
| | Average ES salary | $0 | $0 | $0 |
|---|
| | Average GM/GS grade | 12.1 | 12.1 | 0.0 |
|---|
| | Average GM/GS salary | $114 | $114 | $0 |
|---|
| | Average salary, grade established by act of July 1, 1944 (42 U.S.C. 207) | $163 | $168 | $5 |
|---|
| | Average salary of ungraded positions | $191 | $191 | $0 |
|---|
| Object Classes | FY 2019 Enacted | FY 2020 President's Budget | FY 2020 +/- FY 2019 |
|---|
| | Personnel Compensation: | | | |
|---|
| 11.1 | Full-time permanent | 4,727 | 4,745 | 18 |
|---|
| 11.3 | Other than full-time permanent | 788 | 791 | 3 |
|---|
| 11.5 | Other personnel compensation | 138 | 138 | 1 |
|---|
| 11.7 | Military personnel | 424 | 438 | 14 |
|---|
| 11.8 | Special personnel services payments | 58 | 59 | 0 |
|---|
|
11.9 |
Subtotal, Personnel Compensation |
$6,135 |
$6,171 |
$36 |
|---|
| 12.1 | Civilian personnel benefits | 2,027 | 2,065 | 38 |
|---|
| 12.2 | Military personnel benefits | 238 | 246 | 8 |
|---|
| 13.0 | Benefits for former personnel | 0 | 0 | 0 |
|---|
| |
Subtotal Pay Costs |
$8,400 |
$8,482 |
$82 |
|---|
| 21.0 | Travel and transportation of persons | 448 | 368 | -80 |
|---|
| 22.0 | Transportation of things | 2 | 2 | 0 |
|---|
| 23.1 | Rental payments to GSA | 0 | 0 | 0 |
|---|
| 23.2 | Rental payments to others | 0 | 0 | 0 |
|---|
| 23.3 | Communications, utilities and miscellaneous charges | 81 | 81 | 0 |
|---|
| 24.0 | Printing and reproduction | 0 | 0 | 0 |
|---|
| 25.1 | Consulting services | 0 | 0 | 0 |
|---|
| 25.2 | Other services | 4,923 | 4,123 | -800 |
|---|
| 25.3 | Purchase of goods and services from government accounts | 7,757 | 7,245 | -511 |
|---|
| 25.4 | Operation and maintenance of facilities | 150 | 0 | -150 |
|---|
| 25.5 | Research and development contracts | 171 | -774 | -945 |
|---|
| 25.6 | Medical care | 0 | 0 | 0 |
|---|
| 25.7 | Operation and maintenance of equipment | 9 | 9 | 0 |
|---|
| 25.8 | Subsistence and support of persons | 1 | 1 | 0 |
|---|
|
25.0 |
Subtotal, Other Contractual Services |
$13,010 |
$10,603 |
-$2,407 |
|---|
| 26.0 | Supplies and materials | 92 | 45 | -47 |
|---|
| 31.0 | Equipment | 448 | 98 | -350 |
|---|
| 32.0 | Land and structures | 0 | 0 | 0 |
|---|
| 33.0 | Investments and loans | 0 | 0 | 0 |
|---|
| 41.0 | Grants, subsidies and contributions | 55,627 | 47,555 | -8,073 |
|---|
| 42.0 | Insurance claims and indemnities | 1 | 1 | 0 |
|---|
| 43.0 | Interest and dividends | 0 | 0 | 0 |
|---|
| 44.0 | Refunds | 0 | 0 | 0 |
|---|
| |
Subtotal, Non-Pay Costs |
$69,709 |
$58,753 |
-$10,956 |
|---|
| |
Total Budget Authority by Object Class |
$78,109 |
$67,235 |
-$10,874 |
|---|
[Top]
Salaries and Expenses
(Dollars in thousands)
| Object Classes | FY 2019 Enacted | FY 2020 President's Budget | FY 2020 +/- FY 2019 |
|---|
| Personnel Compensation: | | | |
|---|
| Full-time permanent (11.1) | $4,727 | $4,745 | $18 |
|---|
| Other than full-time permanent (11.3) | 788 | 791 | 3 |
|---|
| Other personnel compensation (11.5) | 138 | 138 | 1 |
|---|
| Military personnel (11.7) | 424 | 438 | 14 |
|---|
| Special personnel services payments (11.8) | 58 | 59 | 0 |
|---|
|
Total Personnel Compensation (11.9) |
$6,135 |
$6,171 |
$36 |
|---|
| Civilian personnel benefits (12.1) | $2,027 | $2,065 | $38 |
|---|
| Military personnel benefits (12.2) | 238 | 246 | 8 |
|---|
| Benefits to former personnel (13.0) | 0 | 0 | 0 |
|---|
|
Subtotal, Pay Costs |
$8,400 |
$8,482 |
$82 |
|---|
| Travel and transportation of persons (21.0) | $448 | $368 | -$80 |
|---|
| Transportation of things (22.0) | 2 | 2 | 0 |
|---|
| Rental payments to others (23.2) | 0 | 0 | 0 |
|---|
| Communications, utilities and miscellaneous charges (23.3) | 81 | 81 | 0 |
|---|
| Printing and reproduction (24.0) | 0 | 0 | 0 |
|---|
|
Other Contractual Services: | | | |
|---|
| Consultant services (25.1) | 0 | 0 | 0 |
|---|
| Other services (25.2) | 4,923 | 4,123 | -800 |
|---|
| Purchases from government accounts (25.3) | 5,049 | 4,483 | -566 |
|---|
| Operation and maintenance of facilities (25.4) | 150 | 0 | -150 |
|---|
| Operation and maintenance of equipment (25.7) | 9 | 9 | 0 |
|---|
| Subsistence and support of persons (25.8) | 1 | 1 | 0 |
|---|
|
Subtotal Other Contractual Services |
$10,131 |
$8,615 |
-$1,516 |
|---|
| Supplies and materials (26.0) | $92 | $45 | -$47 |
|---|
|
Subtotal, Non-Pay Costs |
$10,754 |
$9,111 |
-$1,643 |
|---|
|
Total, Administrative Costs |
$19,154 |
$17,593 |
-$1,561 |
|---|
[Top]
Detail of Full-Time Equivalent Employment (FTE)
| OFFICE/DIVISION | FY 2018 Final | FY 2019 Enacted | FY 2020 President's Budget |
|---|
| Civilian | Military | Total | Civilian | Military | Total | Civilian | Military | Total |
|---|
| Division of International Epidemiology and Population Studies | Direct: | 3 | - | 3 | 3 | - | 3 | 3 | - | 3 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 3 | - | 3 | 3 | - | 3 | 3 | - | 3 |
|---|
| Division of International Relations | Direct: | 5 | 1 | 6 | 6 | 1 | 7 | 6 | 1 | 7 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 5 | 1 | 6 | 6 | 1 | 7 | 6 | 1 | 7 |
|---|
| Division of International Science Policy, Planning and Evaluation | Direct: | 8 | - | 8 | 8 | - | 8 | 8 | - | 8 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 8 | - | 8 | 8 | - | 8 | 8 | - | 8 |
|---|
| Division of International Training and Research | Direct: | 10 | - | 10 | 11 | - | 11 | 11 | - | 11 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 10 | - | 10 | 11 | - | 11 | 11 | - | 11 |
|---|
| Office of Administrative Management | Direct: | 15 | - | 15 | 16 | - | 16 | 16 | - | 16 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 15 | - | 15 | 16 | - | 16 | 16 | - | 16 |
|---|
| Office of the Director | Direct: | 15 | 1 | 16 | 15 | 1 | 16 | 15 | 1 | 16 |
|---|
| Reimbursable: | - | - | - | - | - | - | - | - | - |
|---|
| Total: | 15 | 1 | 16 | 15 | 1 | 16 | 15 | 1 | 16 |
|---|
| TOTAL | 56 | 2 | 58 | 59 | 2 | 61 | 59 | 2 | 61 |
|---|
| Includes FTEs whose payroll obligations are supported by the NIH Common Fund. |
| FTEs supported by funds from Cooperative Research and Development Agreements. | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
|---|
| Fiscal Year | Average GS Grade |
|---|
| 2016 | 11.7 |
|---|
| 2017 | 12.0 |
|---|
| 2018 | 12.0 |
|---|
| 2019 | 12.1 |
|---|
| 2020 | 12.1 |
|---|
[Top]
Detail of Positions
[Note 6]
| Grade | FY 2018 Final | FY 2019 Enacted | FY 2020 President's Budget |
|---|
| Total, ES Positions | 0 | 0 | 0 |
|---|
| Total, ES Salary | 0 | 0 | 0 |
|---|
| GM/GS-15 | 8 | 8 | 8 |
|---|
| GM/GS-14 | 16 | 18 | 18 |
|---|
| GM/GS-13 | 7 | 9 | 9 |
|---|
| GS-12 | 7 | 7 | 7 |
|---|
| GS-11 | 2 | 2 | 2 |
|---|
| GS-10 | 0 | 0 | 0 |
|---|
| GS-9 | 2 | 2 | 2 |
|---|
| GS-8 | 1 | 1 | 1 |
|---|
| GS-7 | 7 | 7 | 7 |
|---|
| GS-6 | 1 | 1 | 1 |
|---|
| GS-5 | 0 | 0 | 0 |
|---|
| GS-4 | 0 | 0 | 0 |
|---|
| GS-3 | 1 | 1 | 1 |
|---|
| GS-2 | 0 | 0 | 0 |
|---|
| GS-1 | 0 | 0 | 0 |
|---|
| Subtotal | 52 | 56 | 56 |
|---|
| Grades established by Act of July 1, 1944 (42 U.S.C. 207) | 0 | 0 | 0 |
|---|
| Assistant Surgeon General | 0 | 0 | 0 |
|---|
| Director Grade | 2 | 1 | 1 |
|---|
| Senior Grade | 1 | 1 | 1 |
|---|
| Full Grade | 0 | 0 | 0 |
|---|
| Senior Assistant Grade | 0 | 0 | 0 |
|---|
| Assistant Grade | 0 | 0 | 0 |
|---|
| Subtotal | 3 | 2 | 2 |
|---|
| Ungraded | 3 | 3 | 3 |
|---|
| Total permanent positions | 55 | 58 | 58 |
|---|
| Total positions, end of year | 58 | 61 | 61 |
|---|
| Total full-time equivalent (FTE) employment, end of year | 58 | 61 | 61 |
|---|
| Average ES salary | 0 | 0 | 0 |
|---|
| Average GM/GS grade | 12.0 | 12.1 | 12.1 |
|---|
| Average GM/GS salary | 113,062 | 114,187 | 114,187 |
|---|
[Top]
Notes
Note 1: Excludes the following amounts (in thousands) for reimbursable activities carried out by this account:
FY 2018 - $9,476
FY 2019 - $8,973
FY 2020 - $8,973
Note 2: All items in italics and brackets are non-add entries.
Note 3: Includes FTEs whose payroll obligations are supported by the NIH Common Fund.
Note 4: Budget Estimate to Congress includes mandatory financing.
Note 5: Includes FTEs whose payroll obligations are supported by the NIH Common Fund.
Note 6: Includes FTEs whose payroll obligations are supported by the NIH Common Fund.
[Top]