Considering culture when providing cancer treatment
January/February 2011 | Volume 10, Issue 1
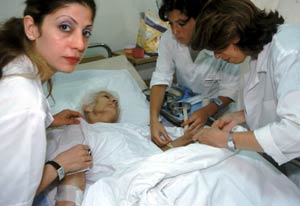
Photo by Alan Gignoux/World Bank
Different cultures in the Middle East have different
views on palliative care, treatment for patients with
serious or life-threatening conditions.
By Elia Ben-Ari
One of the hardest tasks an oncologist faces is telling children with cancer and their families that there is no longer hope of a cure and that the time has come to discuss end-of-life care. For Dr. Myriam Weyl Ben-Arush, head of pediatric oncology at Rambam Medical Center in Haifa, Israel, this task is complicated by the fact that her young patients may be Israeli or Palestinian; Jewish, Muslim, Christian or Druze; religious or nonreligious.
Working effectively in cross-cultural situations such as this is known as cultural competence. In medicine, cultural competence means providing health care services that are respectful of and responsive to the health beliefs, practices and cultural and linguistic needs of diverse patients.
"In the area of palliative care, culture comes into it in a big way," said Dr. Joe Harford, director of international affairs at the NIH's National Cancer Institute. "Different cultures have different views of life, death and pain - and those need to be appreciated."
Palliative care improves the quality of life for patients who have a serious or life-threatening disease and is more effective when provided early.
Harford's office oversees the Middle East Cancer Consortium (MECC), a partnership between the United States and the health ministries of Cyprus, Egypt, Israel, Jordan, the Palestinian Authority and Turkey. In 2005, an effort was begun to build capacity for palliative care.
"The project was established to raise awareness of the palliative care problems shared by all MECC members," said the consortium's director, Dr. Michael Silbermann of Haifa. "It is based on identifying common ground across cultures and relying on their shared interest in establishing palliative care services, as a basis for developing dialogue and cooperation on sustainable cancer care in both hospitals and the communities."
As part of this effort, the consortium has conducted workshops and training. One of the goals is to overcome the fear of opioids, which is a major barrier to providing adequate pain management for cancer patients. The initiative also addresses the needs of children through a group chaired by Dr. Aziza Shad, director of pediatric oncology at Georgetown University Hospital in Washington, D.C.
"No matter what culture you come from, death is the same for everyone. What is important is how you accept it and deal with it," said Shad. "The differences lie in how the family hierarchy works, and who decides how much information on prognosis or end-of-life should or should not be given to the family members or the dying child."
If caregivers don't tell the truth, Ben-Arush explained, "the child will lose his belief in the staff, and he won't cooperate any more…and he will suffer much more, because we need the child [to] explain to us how we can help him."
Ben-Arush noted that it's somewhat easier to talk about death with a Druze family that believes in reincarnation or an Arab Christian family whose child believes in heaven. By contrast, she said, "it is much more difficult for Jewish families to accept that there is no more treatment." They are more likely to ask for experimental therapies for their child and less likely to sign a do-not-resuscitate order, she added.
MECC leaders are now working to introduce basic guidelines for palliative care in the Middle East. After five years of effort, the project is starting to bear fruit.
All articles in the special Focus on Cancer section were developed by the National Cancer Institute and originally published in the NCI Cancer Bulletin and were edited for space. View the full versions of the
November 30, 2010 NCI Cancer Bulletin Special Issue: Global Collaboration.
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.