Scientific findings by NIH-funded studies featuring former AITRP trainees
July / August 2012 | Volume 11, Issue 4
Many scientific findings have resulted from NIH-funded studies that feature former trainees of Fogarty's AIDS International Training and Research Program (AITRP).
Treatment as prevention
A study showed that if patients take antiretroviral drugs as soon as possible after diagnosis, they are 96 percent less likely to infect their HIV-negative heterosexual partner than if they wait until the virus climbs to a specific concentration in their blood. The study involved clinical trials in five sub-Saharan African countries, Brazil, India, Thailand and the U.S. The finding was named Breakthrough of the Year by Science magazine in 2012. As a result, the WHO updated its guidelines to recommend that patients begin antiretroviral therapy immediately after diagnosis.
Circumcision
Mounting observations in HIV patients suggested that circumcised males might be less susceptible to catching the HIV virus than uncircumcised males. Former AITRP trainees in Uganda’s Rakai district conducted studies that confirmed male circumcision reduces HIV incidence. This discovery prompted the WHO to recommend circumcision as a way to help curb HIV infection in high-risk populations.
Cervical cancer
HIV-infected women are more susceptible to infection with the HPV virus that causes cervical cancer, but many cases are diagnosed too late. To see if HIV-positive women in Kenya could undergo low-cost HPV screening during clinic visits, researchers including a former AITRP trainee and an NIH-sponsored researcher investigated the situation. They found 87 percent of women agreed to HPV screening and about 7 percent needed treatment. Other low-resource countries, such as Cambodia, are adopting similar HPV screening recommendations for women with HIV and other high-risk factors.
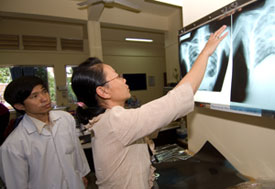
Photo by David Snyder for Fogarty/NIH
Research by Fogarty trainees has uncovered
how HIV and co-infections interface, leading to
earlier screening and treatment for infections
such as tuberculosis, cervical cancer and malaria.
Tuberculosis co-infection
To determine how often HIV and tuberculosis coexist and how severe the problem of multidrug resistance is in rural Kenya, researchers - including former AITRP trainees - developed a house-to-house survey that uses cough monitors. The technique has since been replicated in other countries.
Discordant couples
A large survey in Uganda revealed that HIV prevalence had leveled off, so researchers there investigated the predominant way HIV was being transmitted. They found it was no longer via casual relationships but rather occurred in established relationships. They published their findings in seminal journal articles, which led to changes in prevention strategies in Uganda and other countries.
Antiretroviral adherence
When antiretroviral drugs arrived, some potential donors questioned whether patients in low-resource, low-education settings could follow the regimen of multiple drugs to be taken at precise times each day. AITRP trainees in Port-au-Prince, Haiti, helped conduct a study that showed patients there adhered to the drug regimen as effectively as patients in New York City.
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.