Researchers slow HIV spread among drug users in Vietnam
July / August 2015 | Volume 14, Issue 4
Photo by Abdullah Amir, courtesy of WHO/SEARO
Prevention research helped Vietnam reduce the spread of HIV from
drug users to the wider population, researchers report.
Early in the HIV/AIDS epidemic, fear was high in Vietnam that the virus would spread from drug injecting populations into the wider community. Health authorities had little scientific data to guide their prevention efforts, until researchers funded by the National Institute on Drug Abuse (NIDA) and Fogarty proposed studies to see what might work. Several decades and many discoveries later, HIV in Vietnam is considered to be under control.
"The prevalence of HIV was as high as 60 percent in some provinces among people who inject drugs, and there was not very much in the way of harm reduction interventions going on," said NIDA grantee Dr. Theodore Hammett, of Abt Associates. This epidemic was driven by three key factors: the country's location on a major heroin trafficking route from the Golden Triangle poppy growing region, rising income levels and strong social stigma that makes people who inject drugs harder to reach with prevention information and treatment options.
Hammett and his team targeted the Vietnam-China border region, implementing a peer outreach model in three high-risk communities. They recruited and trained former and current injectors, who then communicated with peers via discussions, meetings and brochures about safe injecting and sex practices. These peer educators also distributed free needles, syringes, condoms and pharmacy vouchers for fresh supplies. They also collected discarded drug paraphernalia, protecting the community from accidental infection and softening their hostility toward drug users. The study documented dramatic declines in HIV prevalence, for instance, down from 51 to 18 percent in one province, with more modest drops in two others. The government then introduced versions of the program elsewhere in the country.
"The generalized epidemic in Vietnam never happened," Hammett said. Latest UNAIDS data put HIV prevalence at 0.4 percent. He added, "It was not entirely a result of our project, but we helped."
Other studies have likewise produced important findings to guide interventions in high-risk communities, such as that fear of social stigma can exacerbate risk-taking after an HIV diagnosis and the extent to which providing sterile syringes can help prevent spread of HIV and other pathogens.
Local drug practices require study
Drug users sometimes develop local customs - designed to avoid detection or amplify their high - that can elevate risk. "The behavioral practices that are used to prepare and inject drugs vary much more widely than is commonly recognized in the public health literature," reported Dr. Michael Clatts, of the University of Puerto Rico. "This kind of research can inform local prevention programming."
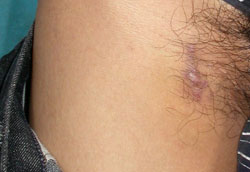
Photo by Dr. Michael Clatts
Some Vietnamese drug users create soft tissue
sacs, like this one in a man's groin, to facilitate
quick injection.
In a NIDA-supported project to examine the influences driving drug use in Vietnam, Clatts and his colleagues discovered some users cultivate a bulge of elastic collagen, or sac, on their skin near a vein, using it as a portal to deliver injected drugs. In Vietnam, the penalty for repeated arrest for heroin possession includes mandated detoxification and extended incarceration, so injectors are anxious to prepare and insert the purchased dose quickly - via direct access to a vein. The injectors also claim that sacs protect their veins when they cannot obtain heroin and resort to the caustic substance Promethazine to ward off withdrawal symptoms. Female sex workers say portals are easier to conceal from their clients and police than puncture marks.
The study showed injectors using sacs took heroin more frequently - two to five times daily - than before and although their rate of HIV infection was similar to injectors without sacs, they shared syringes more often and reported higher levels of hepatitis B infection and pneumonia. The habit is now fairly common in young injectors in Hanoi and has been observed as far away as London. Clatts urged further research to clarify how the sacs might promote the spread of HIV and other pathogens, develop new approaches to deter the habit, and encourage community-based alternatives to the current policing system.
Investigating another serious disease among Vietnamese intravenous drug users, Clatts' team revealed it took drug users only 1.2 years, on average, from the time they started to inject until they acquired the hepatitis C virus. This discovery emphasizes the narrow window available for prevention measures. Currently, almost half the drug injectors harbor this initially symptomless virus and, aside from its health risks, co-infection with HIV raises the risk of poor health outcomes and can curtail HIV treatment options. Approaches should be developed targeting new heroin users, designed to delay onset of injecting and provide information on safe injection practices, Clatts suggested.

Photo by Henrica Jansen, courtesy of Photoshare
A billboard for an HIV/AIDS prevention campaign in Vietnam promotes
condoms and fidelity and discourages unsafe injections.
Scientists investigate stigma's role
Drug users, commonly subjected to stigma for their habit, face additional marginalization if they are also identified as having HIV. The fear of stigma can discourage them from seeking medical attention, exacerbate mental health problems and foster a number of infectious diseases, studies have shown. Dr. Vivian Go, of the University of North Carolina, found that in Vietnam, with its Confucian emphasis on the family's importance over the individual, the impact of stigma often is not only personal but extends to relatives. An HIV diagnosis might push a person to self-isolation and suicide as a means to protect family members.
To learn more about secondary stigma and how to intervene, Go and her team interviewed 25 male intravenous drug users on their thoughts and experiences after hearing they had HIV. Almost everyone cited concern about the emotional impact on their wives, children or parents. Many were also worried about their family's economic well-being, for instance, if tenants of a family property decided to leave because of the association with HIV.
"Men are supposed to support their family but when they inject drugs, they cannot. It is a huge part of marginalization, a huge loss of face," said Go. "Much of the problem is internalized stigma, some real, some perceived. It can prevent them from seeking treatment."
Several men reported they had contemplated suicide to prevent the community learning about their disease, planning to time the act before they became visibly sick with an AIDS-related illness. They said these thoughts were not due to depression, but rather to protect their loved ones from stigma. They also withdrew as a protective step, although they craved family support. Self-isolation has been shown to undermine coping abilities and fuel unsafe injecting and sex behaviors.
"Secondary stigma is a profound concern," the research team wrote in its report. Their analysis was part of a broader study on reducing high-risk injecting and sexual behaviors in Vietnam, funded by NIDA and Fogarty. The scientists suggested that successful HIV prevention interventions "must acknowledge the importance of family in individual decisions about HIV health-seeking behaviors and disclosure."
Efforts to prevent new HIV infections continue to grow in Vietnam, with policymakers guided by evidence from these and other global health studies. "The government has looked to research to provide the evidence base for guiding their policies," Go said.
Just in May, the government directed that all people who inject drugs or are otherwise part of a key at-risk population receive antiretroviral treatment as soon as they are diagnosed as HIV positive, regardless of their CD4-cell count, which is used as an indication of how the immune system is fending off the virus. This policy is more aggressive than the WHO's current recommendation. "This is a great step," Hammett noted. "We hope it will be fully implemented."
More Information
- Learn more about the NIDA International Program and the annual NIDA International Forum.
- Vietnam HIV and AIDS data from UNAIDS
- Efficacy of a multi-level intervention to reduce injecting and sexual risk behaviors among HIV-infected people who inject drugs in Vietnam: a four-arm randomized controlled trial. PLoS One, May 2015
- Variations in the role of social support on disclosure among newly diagnosed HIV-infected people who inject drugs in Vietnam. AIDS and Behavior, May 2015
- Individual-level socioeconomic status and community-level inequality as determinants of stigma towards persons living with HIV who inject drugs in Thai Nguyen, Vietnam. Journal of the International AIDS Society, November 2013
- Controlling HIV epidemics among injection drug users: eight years of cross-border HIV prevention interventions in Vietnam and China. PLoS One, August 2012
- Perceptions of community- and family-level injection drug user (IDU)- and HIV-related stigma, disclosure decisions and experiences with layered stigma among HIV-positive IDUs in Vietnam. AIDS Care, July 2012
- Perceptions of IDU and HIV related stigma within the community and the family, disclosure decisions and experiences with layered stigma among HIV positive injection drug users in Vietnam. AIDS Care, February 2012
- Accelerated transition to injection among male heroin initiates in Hanoi, Vietnam: implications for early harm reduction interventions. Journal of Community Health, December 2011
- Influence of perceived secondary stigma and family on the response to HIV infection among injection drug users in Vietnam. AIDS Education and Prevention, December 2010
- Prevalence and incidence of HCV infection among Vietnam heroin users with recent onset of injection. Journal of Urban Health, March 2010
- Reducing HIV infection among new injecting drug users in the China-Vietnam cross border project. AIDS, December 2007
- Novel heroin injection practices: implications for transmission of HIV and other bloodborne pathogens. American Journal of Preventive Medicine, June 2007
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.