Focus: Using implementation science to reduce mother-to-child HIV transmission
July / August 2016 | Volume 15, Number 4
While the knowledge exists to prevent mother-to-child transmission of HIV, as many as 150,000 new infections occur in newborns every year, mostly in developing countries. A team of scientists and program managers, led by the NIH, has been studying a variety of implementation science approaches to preventing mother-to-child transmission (PMTCT) and has published the results in a
16-article supplement to the
Journal of Acquired Immune Deficiency Syndromes.
"We have the tools at this moment to further decrease the incidence of new infections, but we need to apply these tools more effectively to reach the undiagnosed and untreated mothers," Fogarty Director, Dr. Roger I. Glass, and U.S. Global AIDS Coordinator, Dr. Deborah L. Birx, wrote in a
foreword to the supplement.

Photo by Dina Patel/HealthySunrise Foundation
A study showed that involving men in prenatal care improves outcomes
for mothers and infants, and increases the likelihood that the male
partners will be tested for HIV.
The open-access articles are focused on ways that implementation science - the emerging field in which scientists study how to integrate research findings and other evidence-based practices into routine care and services - can support efforts to eliminate pediatric HIV.
PMTCT involves a cascade of factors that are inherently complex, crossing numerous biological phases for women and their infants, and requires deployment of multiple services within the health sector, the authors noted. Some studies used systems engineering approaches to examine treatment workflow, identify bottlenecks and gaps, task shifting and other issues. Facility-level problems were considered, including drug shortages, overburdened staff, lack of service integration, insufficient mentoring, and poor patient-provider interactions. The scientists also identified domestic violence, abandonment and stigma as key barriers.
The authors reported on the effectiveness of a variety of interventions:
- Collaborating with churches to invite pregnant women to "baby showers," which included HIV testing and gifts, was nearly twice as effective for screening and recruiting for treatment those who tested positive for HIV, than were invitations to clinic visits providing the same benefits.
- Offering HIV testing and counseling for breastfeeding, family planning and other issues in the homes of study participants made it twice as likely the male partners - who often report feeling uncomfortable making clinic visits but are key to reducing HIV transmission - would be tested.
- Training lay volunteers or "feeding buddies," to provide information about breastfeeding, infant health and HIV treatment protocols that may diminish the damaging impact of stigma on HIV-positive mothers and allow them to safely feed their children and adhere to WHO guidelines, which recommend exclusive breastfeeding, antiretroviral therapy and early infant testing.
- Providing cash incentives for prenatal clinic visits appeared to help keep women in care, but did not boost adherence to antiretroviral therapy.
- Initiating drug therapy during pregnancy caused rapid declines in viral load, but more than 95 percent of women studied reported at least one side effect before delivery, which may lower adherence.
- Deploying a point-of-care test for infant diagnosis of HIV using a portable, battery-operated device may result in more timely initiation of drug therapy, decreasing the number of children who may be diagnosed with HIV weeks or months after birth, lost to-follow-up and never receive care.
- Administering pre-exposure prophylaxis (PrEP) for HIV prevention among pregnant and breastfeeding women in sub-Saharan Africa is likely cost-effective, economic modeling indicates.
Researchers and policymakers from the U.S. and Africa who contributed to the supplement articles were part of the
PMTCT Implementation Science Alliance, created and supported by the NIH and the President's Emergency Plan for AIDS Relief (PEPFAR), to investigate the role implementation science can play in enhancing the quality and effectiveness of PMTCT efforts. Research projects described in the supplement were funded by NIH grants from the
Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), National Institute of Allergy and Infectious Diseases (NIAID), National Institute of Mental Health (NIMH) and the Office of Research on Women's Health (ORWH).
Some Barriers in Preventing Mother-to-Child HIV Transmission
- Lack of reproductive health information and services for adolescents
- Poor integration of family planning into health care services
- Lack of effective and efficient early infant diagnostic services
- Low uptake of prenatal, delivery and post-natal care services
- Poor understanding of factors that impact retention of mother-infant pairs in care
- Too few studies of community-based services to improve retention in care
- Inequitable distribution of health care workers in rural vs. urban areas
- Poor male partner involvement, too few studies on how to engage men
- Inadequate integration of PMTCT services in maternal and child health care
- Lack of coordination between government, implementers and researchers
- Gaps in local health financing for PMTCT implementation and research
- Underutilization of traditional birth attendants and private hospitals
Source:
Identifying and Prioritizing Implementation Barriers, Gaps, and Strategies Through the Nigeria Implementation Science Alliance: Getting to Zero in the Prevention of Mother-to-Child Transmission of HIV,
JAIDS Supplement, June 30, 2016 (online)
The NIH-PEPFAR Alliance was led by Fogarty's
Center for Global Health Studies. In addition to the funders, other participants in the Alliance include the Office of AIDS Research at NIH, along with outside agencies including the Centers for Disease Control and Prevention (CDC), the Elizabeth Glaser Pediatric AIDS Foundation, South Africa's Anova Health Institute, the United States Agency for International Development (USAID) and the WHO.
The Alliance was "a kind of ‘living laboratory,' providing an exciting opportunity to explore how enabling tools can help to effectively build, strengthen and nurture interactions between researchers, program implementers and policy makers, and whether this kind of model can catalyze positive results for implementation science and global health," Fogarty's Dr. Rachel Sturke and colleagues wrote in an
article introducing the studies.
Despite enormous successes in PMTCT, important challenges remain, the Alliance members noted. They have identified priority areas for future study, including how to link HIV-positive infants into early treatment, improve models for retention and adherence of children receiving antiretrovirals, and prioritize locally driven research questions and processes that engage end users throughout.
"Continuing to find innovative ways to foster collaboration of implementation science researchers with decision makers and program implementers will be critical to speed the translation of effective PMTCT interventions in the local context and health system programs," the authors conclude.
Although the incidence of pediatric HIV has dropped dramatically in many parts of sub-Saharan Africa, there are some places where it remains common. In 2015, PEPFAR supported testing for almost 15 million pregnant women, with 850,000 of them found to be HIV-positive and 831,000 started on ART. Yet, several hundred thousand babies continue to be born with HIV each year and scientists are studying implementation science approaches to further reduce that number.

Photo by Dina Patel/
HealthySunrise Foundation
An expectant mother in Nigeria is tested
for HIV while attending a "baby shower,"
at a church, where free HIV tests and
prenatal care are offered.
Providing care outside the clinic
By reaching pregnant women in their homes or churches, researchers discovered they can
increase the number who are tested for HIV and begin treatment, as well as lower the number of infants who become infected. In a Nigerian community where 90 percent of the population attends church, researchers enlisted the help of congregation leaders to hold monthly "baby showers," where women and their partners were offered free HIV screenings, counseling and gifts. Half of the 3,002 pregnant women in the study were assigned to attend the baby showers, while the other half were encouraged to seek prenatal care at clinics, where similar benefits were provided at no cost. Ninety-two percent of the women who went to the church baby showers were screened for HIV, compared to 55 percent of women in the control group, the researchers found. Women who attended the baby showers were also six times more likely than the control group to start ART if they were found to be HIV-positive.
Engaging male partners in the process
Increasing the
rate at which men are tested for HIV and involved in prenatal care was a priority for one group of researchers working in Kenya. Only 4.5 percent of men with pregnant partners were screened for HIV in 2013, versus 88 percent of expectant mothers. Couples in this study were assigned either to receive a home visit - during which they were screened for HIV and given advice on childbirth, the postnatal period and prevention of HIV transmission - or invited to attend a clinic where they would be tested together for HIV. The researchers found men in the home visit group were more than twice as likely to be screened for HIV as men who were invited to the clinic, and women in the home visit group were twice as likely to know their partner's HIV status as those in the clinic group.
A separate study by the same researchers looked at the
cost-effectiveness of home-based HIV testing. The researchers projected that if 60 percent of male partners were screened for HIV at home, nearly 7,000 infections and 2,600 deaths would be averted. They found home visits to be cost-effective, and said they could be made even more affordable by task shifting responsibilities from medical staff to community health workers.
Using mentors to promote breastfeeding and retention
In a study in South Africa,
new mothers were encouraged to choose a "feeding buddy" - someone trained in all aspects of breastfeeding, infant health and the importance of taking ART. The researchers hypothesized that women with a feeding buddy would be more likely to still be breastfeeding at six months than those without. They found that feeding buddies played an unexpected but important role - as confidantes to women who felt stigmatized because of their HIV status. Feeding buddies improved women's ability to accept and cope with their HIV status, and reduced feelings of social isolation, which meant a woman would be less likely to drop out of care.
Meanwhile,
lay counsellors called
mama mshauri (mother mentors) are being used in Kenya to try to retain women in care.
Mama mshauri are community workers who are trained to provide services to women, including PMTCT health education, and voice and text message appointment reminders.
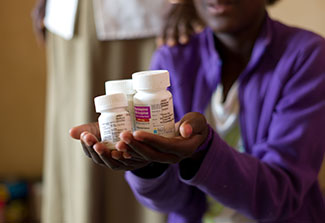
© UNICEF/UNI103221/Nesbitt
A teenaged girl in Botswana in 2010 holds up the
antiretroviral medicines she has been taking since she was
diagnosed with HIV four years earlier. Antiretroviral therapy
(ART) is effective in reducing HIV-related illnesses and death,
but many people do not stick with the therapy.
Studying antiretroviral therapy during pregnancy
Because rates of HIV acquisition may double during pregnancy and breastfeeding among women in sub-Saharan Africa, scientists studied whether
pre-exposure prophylaxis (PrEP) with antiretrovirals would be a cost-effective approach. If the mother becomes infected during pregnancy or breastfeeding, the risk of infant infection is almost 23 percent, studies have shown. Scientists who looked at the cost-effectiveness of administering PrEP to at-risk pregnant women found that the treatment averted 3 percent of HIV infections but resulted in 7 percent more preterm births. However, when the scientists weighed the cost of caring for preterm infants against the cost and benefits of PrEP, they concluded that giving the preventive treatment to pregnant and nursing women would likely be cost-effective.
Meanwhile, scientists in South Africa were concerned that
women's adherence to therapy was "suboptimal." They analyzed data that showed more than 95 percent of women initiating drug therapy during pregnancy reported at least one side effect before delivery. While no single side effect was associated with missed doses, "the total number of side effects experienced was a strong predictor of non-adherence," the study's authors observed.
In Mozambique, which offers lifelong ART under the Option B+ program, researchers have found
high rates - more than 90 percent - of HIV testing and ART initiation, but 90-day retention rates of only 5 to 30 percent. When the researchers analyzed work- and patient-flow at six clinics, they identified several potential causes of the high dropout rate, including long wait times, short consultations and poor counseling. Among the fixes they suggested were shifting part of nurses' workloads, which had increased significantly under Option B+, to community health workers, and following up with patients via home visits and text messages.
Speeding infant diagnosis
Since half of untreated HIV-infected infants die before their second birthday, a research team in Zambia is testing a new
point-of-care diagnostic that produces immediate results to improve the early entry of HIV-positive infants into care. Unlike screening in adults, diagnosis in infants requires specialized lab equipment and highly trained personnel. That means many infants remain without a diagnosis for weeks or months, so treatment is delayed or never begins. The testing platform is portable, battery operated and designed to withstand heavy use - ideal for resource-poor settings.
Testing cash incentives
To improve retention rates in the Democratic Republic of Congo, researchers
paid one group of women a small sum each time they attended a prenatal clinic and agreed to take the prescribed care, while another group received no compensation for clinic attendance. Six weeks after the birth of their babies, 80 percent of HIV-infected women who received the cash incentives were still coming to the clinic, versus nearly 73 percent of women who did not receive money. But while the payments appeared to help keep women in care, they did not boost ART adherence.. Thirty percent of women in both groups did not faithfully take their antiretrovirals - possibly because doing so was not a condition for being paid for each clinic visit.
Task shifting to maximize resources
To assess the impact task-shifting has on patients and medical professionals, mothers and medical staff in northern Nigeria were asked to rate their
satisfaction with PMTCT services delivered either at comprehensive care clinics or clinics offering specialized PMTCT care, where some tasks were delegated to midwives. Mothers who attended the clinic offering specialized care were more satisfied than women assigned to the comprehensive clinics. Providers in both settings were motivated and happy with their compensation and training, but less satisfied with task-shifting.
Using novel tools to analyze approaches
When researchers applied systems engineering theories and tools - including work processes, optimization methods, risk management, and logistics - to
analyze PMTCT programs in Côte d'Ivoire, Kenya and Mozambique, they identified human resources shortages, lack of mentoring and stigma as some of the main barriers to successful implementation. Using the Consolidated Framework for Implementation Research (CFIR) - a method used to assess potential barriers and facilitators in a system - the researchers highlighted key differences between high- and low-performing care facilities, including that high-performers tend to communicate better, which allows them to be more efficient when implementing changes.
Concept mapping - a visual system for organizing and representing knowledge, and depicting the relationship between concepts - was used by another research group to
identify the main areas that influence PMTCT implementation in sub-Saharan Africa. Two components - government commitment and data measurement and collection - consistently ranked highly in the exercise, suggesting that they are key to successful PMTCT program implementation. The study concluded the findings could be used "to inform strategies to optimize PMTCT implementation and services in the field."
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.