mHealth app reduces risks in pregnancy, delivery in LMICs
Volume 20 Number 4
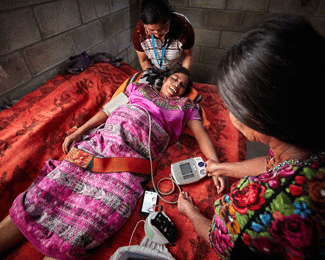 Courtesy of Bryan Watt, Photograpers Without BordersNIH-funded researchers have developed and tested a mobile health screening tool in rural Guatemala that enables midwives to screen pregnant Maya women for complications and make referrals to health care facilities
Courtesy of Bryan Watt, Photograpers Without BordersNIH-funded researchers have developed and tested a mobile health screening tool in rural Guatemala that enables midwives to screen pregnant Maya women for complications and make referrals to health care facilities
Pregnancy and childbirth are especially risky in rural Guatemala where about half of Indigenous Maya women deliver their babies at home with the assistance of midwives. With little capacity to screen for complications—combined with language issues and the systemic discrimination Maya women face navigating health care facilities—the result is higher maternal and infant mortality rates than elsewhere in the country.
NIH-funded researchers have developed and tested a mobile health solution that is helping to change that. By combining a $10 ultrasound device, blood pressure cuff and pulse oximeter that feed directly into a smartphone, Emory University’s Dr. Gari Clifford and colleagues have produced a screening and referral tool that enables midwives to spot issues and make referrals to health care facilities. Working closely with a local organization, the team developed an app to guide low-literacy midwives through a pictographic checklist of common complications. A positive indication triggers automatic communication with an on-call clinical team. Vital sign abnormalities also spur text message alerts. The app includes audio instructions for how to deal with different scenarios recorded in the local Kaqchikel language for those who cannot read.
During a one-year randomized control feasibility study involving about 800 pregnancies, use of the screening app resulted in “a significant increase” in emergency referrals to care facilities and demonstrated the technology was feasible for use in the low-resource setting. The results were so impressive, the tool has been adopted as standard of care and used in several thousand births over the last five years.
.jpg) Source: Martinez et al. (2018)Reproductive HealthThese images show the decision support workflow for the mHealth platform designed to reduce maternal and infant mortality in Guatemala.
Source: Martinez et al. (2018)Reproductive HealthThese images show the decision support workflow for the mHealth platform designed to reduce maternal and infant mortality in Guatemala.
One recent patient diagnosed with pre-eclampsia by a midwife using the mHealth app said she owes her life to the program. Her midwife used the app to connect her with a care navigator from a local organization, who accompanied her to the hospital where she delivered a healthy baby via cesarean section.
The intervention’s success is the result of close collaboration with the local organization, Wuqu' Kawoq (Maya Health Alliance). The Alliance recruited the necessary Guatemalan health care institutions and providers plus midwives to partner on the project. “Our work is important because we are one of the only groups to really understand the social determinants of health for Indigenous communities in rural Guatemala,” said Dr. Peter Rohloff, its chief medical officer and co-investigator. Throughout the study, he built these relationships, navigated the public health regulatory environment and facilitated the participation of the midwives in the design process.
“We’re talking so much about decolonizing global health and shifting power dynamics and I think this is how you do it,” observed co-investigator Dr. Rachel Hall-Clifford, an anthropologist at Emory. “The co-design process— developing the program and the app with the women and implementing it—is so deeply meaningful and essential for creating sustainable programs.”
The project was largely funded by the
Eunice Kennedy Shriver National Institute for Child Health and Human Development through Fogarty’s mHealth program. Since 2013, Fogarty has been working to catalyze mHealth innovation through multidisciplinary research that addresses global health problems, develop an evidence base for mHealth and strengthen research capacity. In Guatemala, 44 midwives were trained to diagnose and monitor key pregnancy complications as defined by the WHO. Several personnel involved received mentorship in research study design, technology development and scientific writing.
The scientists believe the program could be scaled up across Guatemala and holds potential for other low�resource settings. The team is currently building a new collaboration with Morehouse School of Medicine to adapt the program to serve an African American population in Georgia. “In global health, we are eager to get stuff done and start saving lives,” noted Hall-Clifford. “But it’s important to take a breath, and work with stakeholders to build long-term partnerships.”
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.
Related Fogarty Programs
Related World Regions / Countries
Related Global Health Research Topics