Lack of adherence in HIV trial has broad implications
March / April 2015 | Volume 14, Issue 2

Photos courtesy of the Microbicide Trials Network,
University of Pittsburgh and Magee-Womens
Research Institute
Researchers were studying methods to reduce HIV infection
in women at risk.
A large, NIH-supported clinical trial in sub-Saharan Africa aiming to identify the best method to protect women from contracting HIV instead underscored that researchers cannot rely on self-reporting to gauge if study participants are following instructions.
Women assigned to receive antiretrovirals daily via a pill or vaginal gel acquired HIV at a similar rate as those on placebos. When analyzing blood samples, researchers discovered only 28 percent of women had taken the drugs, rather than the 80-90 percent compliance rate participants reported.
"It was pretty shocking," said lead co-investigator Dr. Jeanne M. Marrazzo, of the University of Washington. "We had very little to no clue that the women were not taking the product to that extent." A report on the study was recently published in the New England Journal of Medicine.
The adherence finding has implications for the design of similar randomized controlled trials. "It's probably going to be much more impactful as a negative study than it would have been as a positive study," Marrazzo predicted. "Other trials are now routinely monitoring adherence in real-time, or considering doing this."
The team investigated why women had avoided the medication and found many wanted to hide their trial participation from partners and families to avoid the stigma of being associated with HIV risk. "We heard a lot of stories where they were really anxious about having the study products at home," Marrazzo said.
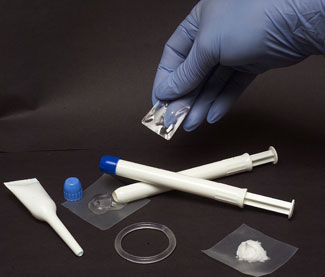
Only 28 percent of study participants actually used the daily
pills or vaginal gel as instructed.
The women were also discomfited by the study's implications that they were vulnerable to catching HIV, because they felt healthy and at low-risk. They nonetheless enrolled, and ensured they remained so, to access free medical care, sexually transmitted disease testing. They also received financial reimbursement, but it was minimal and not considered a motivator, Marrazzo said.
Although disappointing, the results were also enlightening, she observed. "We thought we were studying a biomedical intervention, but really we were studying a multi-component prevention intervention in different communities. It had everything to do with those individual women's lives and challenges and burden of trying to remain HIV negative."
The project involved 5,029 reproductive-age women who were HIV-negative, registered at 15 sites in South Africa, Uganda and Zimbabwe. It is part of a larger effort, the Vaginal and Oral Interventions to Control the Epidemic, or VOICE study, led by the NIH's National Institute of Allergy and Infectious Diseases (NIAID) with support from the National Institute of Child Health and Human Development (NICHD), the National Institute of Mental Health (NIMH), CONRAD and Gilead Sciences, Inc. The VOICE study is being conducted by the Microbicide Trials Network.
The project followed up on several smaller studies in various countries showing that prophylactic antiretroviral drugs could reduce new HIV infections by more than 50 percent in at-risk people adhering to the prescribed regimen. This trial involved different combinations of tenofovir, pills or vaginal gel, and emtricitabine pills, tested against a placebo. All participants received standard HIV risk-reduction counseling, individualized adherence counseling, condoms and hepatitis B immunization.
From the outset, the team was mindful of the need to monitor adherence, so required participants visit the clinics monthly for an interview about their compliance and to return pill bottles, all remaining pills and unused vaginal applicators. Every three months, the women also underwent a computer-assisted self-interview designed to avoid any subjective staff influence. By these measures, adherence appeared high, but 312 women tested newly positive for HIV.
The researchers found that the women most likely to take the drugs as instructed were those with the lowest HIV risk before the trial - they were older, married and had an independent income. In a number of earlier studies with higher adherence rates, participants had more motivation to take the antiretrovirals, for instance couples in which one partner was already infected or pregnant women eager to protect their babies.
Marrazzo said aside from incorporating more blood sampling in trials, researchers are looking at other approaches for HIV drug delivery, such as long-term vaginal rings, implants or injections, which can lessen both the stigma and inconvenience of taking daily medication. "Taking a pill every day is hard, especially if you're young and you feel invulnerable," she said. Moreover, she added, some cultures regard injections as more effective therapy, so more acceptable, than pills. "There's no one size fits all, that's really the answer."
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.