Focus on pain research in LMICs: Scientists use mobile health app to mitigate pain in Nepal
March / April 2020 | Volume 19, Number 2
By Susan Scutti
In Nepal, palliative care services may not be widely available, causing many to suffer unmitigated pain. “During my first trip there in 2004, I was very naive and I saw for the first time what cancer unchecked looks like,” said Dr. Virginia LeBaron of the University of Virginia. “We worked in hospitals there where the only available pain medicines were Tylenol and Motrin.”

Photo courtesy of Arati Ghising Tamang
Fogarty grantee Dr. Virginia LeBaron (left) is
collaborating with local partners in Nepal on a
digital platform.
Since then, Nepal has made significant improvements in the availability of essential pain medicines, such as opioids, and developed evidence-based pain management guidelines that are tailored to meet local needs. But because the guidelines currently exist only on paper, implementation has been inconsistent and there is no way to track how they are being used, LeBaron said. She hopes to change that by developing a digital platform that will provide decision-making support for health providers treating patients experiencing cancer pain, supported by a
two-year Fogarty mobile health grant.
Pain Treatment Guidelines
Mobile App
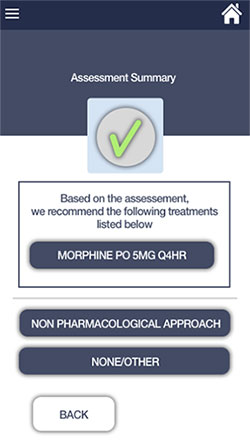
Image courtesy of Hass Software Consulting
Screen shot of pain treatment guidelines
mobile app.
LeBaron is collaborating with local partners, including the
Nepalese Association of Palliative Care (NAPCare), which developed the guidelines. The team began by designing and conducting a survey at four cancer sites in Nepal. Participating nurses, physicians and pharmacists answered questions about their attitudes and knowledge of managing cancer pain, awareness of the NAPCare guidelines, the features they would like in the app and related issues. The responses will help researchers understand potential barriers to cancer pain management and help inform the app's design.
Analysis of the data is still in progress, yet early results indicate that opioids are more consistently available than previously thought. Smartphone use is ubiquitous and health providers are willing to use a mobile app, however some are restricted from using cellphones at work. They should be empowered, said LeBaron, who began her career as an oncology nurse. “Nurses are inherently trained to think holistically about a person and are highly attuned to human suffering and their role in mitigating that.” The current version of the app focuses on healthcare providers but LeBaron hopes to evolve the app’s design to be patient-facing as well, so families can participate in pain management decisions, she added.
Skills learned on the Fogarty project will equip the Nepal team members to initiate and conduct their own independent research projects, LeBaron believes. Meanwhile, her overall app-building model has applicability far beyond Nepal. “Working closely with clinical partners in low- and middle-income countries (LMICs), implementing guidelines that consider the cultural and resource context, and using local surveys to gather feedback are all strategies that can be used in similar settings to improve the delivery of palliative care and cancer pain management,” she said.
Trapped at home due to the coronavirus pandemic, LeBaron is thinking about cancer care in LMICs in new ways. Physical closeness and connection are cultural norms offering strength and a source of comfort, while Nepali institutions manage a huge volume of patients. “Isolation rooms and social distancing, logistically and practically, may be very difficult in many LMICs,” she noted. Her work with oncology nurses there taught her that personal protective equipment is not available when needed. Add to that, there’s “an existing ‘opioid-phobia’ or fear around the use of opioids even when it is legitimate and very necessary,” she said: “Will providers be willing to use morphine with COVID-19 patients if needed to help manage difficulty breathing?” Finally, the pandemic will not stop cancer, and patients will continue to experience severe pain.
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.