Profile: Fogarty Fellow Dr Matchecane Cossa studied surgical quality in Mozambique
November / December 2020 | Volume 19, Number 6
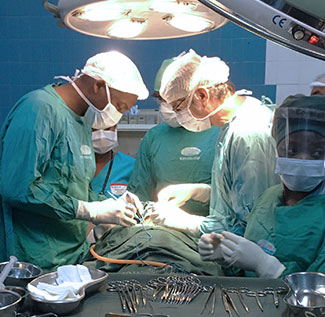
Photo courtesy of Dr. Matchecane Cossa, pictured left
By Susan Scutti
Although non-traditional ‘surgeons’ perform 40% of operations in Mozambique, the mortality rate is comparable to other regions in Southern Africa, according to a study conducted by Fogarty Fellow Dr. Matchecane Cossa. With only one surgeon for about every one million people in Mozambique, nurse technicians are essential. “We can train a nurse to perform surgeries as a way to help people,” explained Cossa. In the research project he conducted during his fellowship, he measured not only the volume but also the quality of surgical care in Mozambique’s 45 district hospitals using standard WHO criteria. He tallied the number of operating rooms, operations, accredited surgeons and anesthesia professionals as well as day of surgery death rates and post-operative in-hospital death rates.
Cossa had recognized the need for this kind of data after being appointed chief of surgery for his country’s health ministry. “When I got there, someone asked me: How many surgeons do you have? How many procedures are performed each year? What are your stats?” Some information existed, but Cossa suspected the numbers might not be reliable, especially for rural areas. He decided, “If I gather this information, it will help me make decisions based on exactly what we have.”
While most surgeons don’t conduct research, Cossa’s mentors inspired him to break this trend. “I always wanted to do research and I had been searching for an opportunity,” said Cossa, who had chosen thoracic surgery as his specialty because Mozamique had no practitioners in that field. Given the country’s high rates of tuberculosis, which can require thoracic surgery, he knew he would be able to make an impact. Once he secured his Fogarty fellowship, he cobbled together a team of medical students and residents working in Maputo along with surgeons across the country. “I convinced them that this was important and I sent them a template so they could collect data for me,” he said. He’d assumed information would be submitted by email or snail mail. Technology challenges meant he received photos of completed surveys via WhatsApp, which then needed to be entered manually into the system.
The study has already influenced policy decisions. The findings showed the health ministry where operating rooms are needed and which provinces require a surgeon. “We have less surgeons by far than the target set by the WHO and we have very few ORs, very few anesthesiologists,” said Cossa. “But the mortality rate is not that high and is similar to Southern African regions.” Surgical death rates of the trained nurses were similar to rates among actual surgeons. “Of course, people would prefer to be operated on by a general surgeon, but the results show that for our country the work of the trained nurses is laudable and very important,” he said.
Another result of the study: Cossa has seen a shift in attitudes of younger surgeons, who now express an interest in conducting research. “When you think about LMICs, you think that it’s quite difficult to get information but it’s always feasible,” said Cossa.
An important benefit of his Fogarty project was the online training. “Every week there were programs, classes, all about research,” he said. Unexpected lessons were learned as well. “Many people think that, when they gather information from the work they’ve done, this data belongs to them and they want to keep it to themselves,” said Cossa. “Through Fogarty, the most important thing I learned is collaboration and cooperation.” As a result, he has since worked with scientists in Peru, the U.S. and Spain.
Cossa’s research also opened his eyes to the limits of health care investment. “We realized the mortality rate is higher in the poorest province,” said Cossa. “It’s not a problem of health services and health personnel - it’s the whole situation. Infrastructure and development of the entire province has to be combined with the development of the health system. You cannot expect good results otherwise.”
Today, when younger surgeons ask about Fogarty, Cossa tells them “go for it, it will help your career,” yet at the same time he cautions that “it takes a lot of time.” The greatest benefit of all is the ability to improve yourself, he said: “You can find what is wrong with what you are doing and change it because you have this collaboration with the entire world. Through research you have the opportunity to develop your career as a health professional.”
Cossa was originally inspired to take up research by UK-based Dr. Peter Bentley and received further encouragement and help analyzing his data from his Fogarty mentors, Dr. Stephen Bickler of UC San Diego and Dr. John Rose of Johns Hopkins University.
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.
Related Fogarty Programs
Related World Regions / Countries