This section responds to the Learning Collaborative’s priority of advancing implementation science. It describes tools to:
- Frame research using validated implementation science methodologies and frameworks.
- Engage communities, policymakers, and program-implementers in identifying locally relevant research questions that are responsive to local health priorities.
The gap between the promise of scientifically proven health interventions and their successful implementation in the real world persists in a wide variety of contexts including neurology and brain disorders. Implementation science (IS) plays an important role in identifying barriers to address these enduring gaps in the translation of evidence into policy and programs. Importantly IS within neurology and brain disorders has the capacity to reduce disparities and provide higher uptake of proven treatments (Vickrey, Hirtz, Waddy, Cheng, & Johnston, 2012). This section describes a set of commonly used implementation science frameworks and includes approaches that bolster researcher interaction with end users of research. Key resources for practice, and training resources for IS are listed in
Resources for Implementation Science Researchers. Developing strong relationships with diverse partners is integral in all of these models and resources for relationship building are also included.
NIH defines IS as the study of methods to promote integration of research findings and evidence into healthcare policy and practice (Fogarty International Center). This emerging, interdisciplinary field lacks consistent terminology (Chambers, Glasgow, & Stange, 2013; Tabak, Khoong, Chambers, & Brownson, 2012). The scientific literature describes a broad landscape of theories, models, and frameworks utilized in IS which can be used to examine the array of questions pursued by IS practitioners to inform the application of new scientific discovery.
Important to all IS frameworks is the distinction between effectiveness and efficacy, as well as the concept of scale-up. IS examines implementation of interventions within the controlled environment of research, testing effectiveness and then pilots that intervention in a local context or scales it up to population level impact testing efficacy. The term effectiveness is used to describe the outcomes of an intervention in a real word context when implemented in situ (Glasgow, Vogt, & Boles, 1999). This is in contrast to the term efficacious, which is used to describe how well the intervention works in the research or optimal setting under conditions that can be very different from the over-burdened and under resourced reality of a public clinic or community-based program.
Moulin and colleagues review the scientific literature on IS and divide the frameworks and models in field into categories according to target innovation and the comprehensiveness of the framework. They identify core components and develop a generic structure that builds on essential core components. The core concepts that they recommend be considered in every implementation endeavor include: those concepts relating to the process of implementation, the innovation itself, the context, influencing factors, strategies, and evaluations (Moulin, Sabater-Hernandez, Fernandez-Llimos, & Benrimoj, 2015). The generic framework depicts these core concepts and their relationships to one another and a diagram is reproduced below in Figure 1. This framework may be most useful in conceptualizing an intervention in terms of core IS components and could be used in conjunction with a model that benefits from a deeper literature base.
Figure 1: Generic Implementation Framework
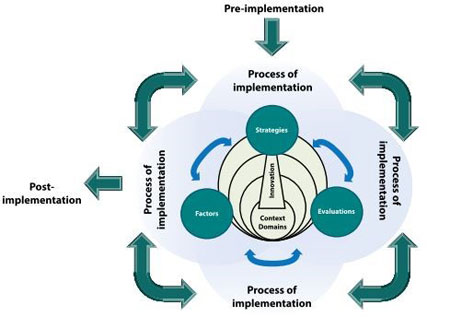
Full description of
Figure 1: Generic Implementation Framework:
Chart shows flow of a generic implementation framework. Top arrow points from
pre-implementation to process of implementation. Overlapping circles show
process of implementation, and depict circular relationships between strategies,
evaluations and factors. They surround concentric circles labeled context domains,
and a box labeled innovations. Arrows show all components work together to
comprise the process of implementation. Final arrow point left to post-
implementation.
Tabak and colleagues provide an comprehensive review of models specifically designed for use by scientific researchers in health (Tabak et al., 2012). Many of these grew out of E. Rogers’ seminal Diffusion of Innovations Theory which describes the ways that innovations diffuse and the role for dissemination in increasing the speed of innovation transfer from scientific research to end users (Nilsen, 2015; Rogers, 1995). Tabak and colleagues identified 61 models for dissemination and/or implementation research with application in community- or organizational-level dissemination. They categorize the models in an extensive table that reflects whether the model relates to dissemination and/or relates to implementation, a rating of flexibility reflecting a continuum of broad and malleable constructs to more fixed operational ones, as well as the level within The Social-Ecological Model addressed by the specific IS model (Tabak et al., 2012).
The set of models described here represent examples of commonly used IS frameworks and include approaches that bolster researcher interaction with end users of research. These models also seem to be the best documented within the neurosciences in LMIC contexts. They include: The Framework for Reach, Effectiveness, Adoption, Implementation, and Maintenance (RE-AIM); Precede-Proceed; Dynamic Sustainability; Practical, Robust Implementation Sustainability Model (PRISM); and Consolidated Framework for Implementation Research (CFIR).
RE-AIM Framework
The RE-AIM Framework conceptualizes public health impact of an intervention as a product of the interaction between five factors: reach, effectiveness, adoption, implementation and maintenance. RE-AIM focuses on reach and representativeness of both participants and settings and fits with systems-based approaches and the social-ecological model (Glasgow et al., 1999). Tabak et al write that this model is more operational than many IS models and inclusive of both dissemination and implementation issues (Tabak et al., 2012). It is most useful for providing an evaluation of interventions that address multiple causes and holistic systems (Glasgow et al., 1999).
Briefly, to define each of the five factors, reach is an individual-level measure of participation and refers to the percentage and risk characteristics of persons who receive or are affected by a policy or program. Adoption refers the proportion and representativeness of settings that adopt a given policy or program. Implementation means the extent to which a program is delivered as intended. And lastly, maintenance measures the extent to which innovations become a relatively stable, enduring part of the behavioral repertoire of an individual, organization or community. Abrams et al argue that the impact (I) of an intervention is the product of the reach (R) and the efficacy (E), or I = R x E (Glasgow et al., 1999).
RE-AIM Example 1
King, D. K., Glasgow, R. E., & Leeman-Castillo, B. (2010). Re-aiming RE-AIM: using the model to plan, implement, and evaluate the effects of environmental change approaches to enhancing population health. American Journal of Public Health, 100(11), 2076-2084.
An example of the application of the RE-AIM frameworks can be found in research by King et al entitled, examining the impact of the built environment on public health (King, Glasgow, & Leeman-Castillo, 2010). They point out the flexibility of this model for different aspects of public health by modifying the definitions of each dimension to describe the built environment. They also offer three detailed options for quantifying RE-AIM into a summary score that may prove useful when presenting evidence to diverse audiences (King et al., 2010).
Precede-Proceed Model
Precede-Proceed is a dominant model in health promotion with a significant body of literature (L. W. Green, 1999). Precede-Proceed is an acronym for Predisposing, Reinforcing and Enabling Constructs in Educational Diagnosis and Evaluation (PRECEDE) – Policy, Regulatory and Organizational Constructs in Educational and Environmental Development (PROCEED). The model offers a detailed process for program planning and evaluation that considers the impact of the organizational and environmental systems on the selected intervention and has been applied in various situations, including cross-cultural programs to change health behavior. It is most useful when planning an intervention and including the evaluative components upfront while providing analysis at every step in the process. The eight phases (some versions have six phases) walk the researcher through situational analysis, development, and finally evaluation of the intervention (Glanz, Rimer, & Viswanath, 2008; L. Green, 2015).
Precede-Proceed Example 1
Colodny, N., Miller, L., & Faralli, M. (2015). The development of a feeding, swallowing and oral care program using the PRECEDE-PROCEED model in an orphanage-hospital in Guatemala. International journal of speech-language pathology, 17(2), 127-137.
Research to improve medical provider skills for swallowing support for children in a Guatemalan orphanage used the Precede-Proceed model. The affected children suffered impaired swallowing due to various health conditions like cerebral palsy and craniofacial malformations. Colodny et al describe an intervention called international academic service-learning (IAS-L), a technique to improve medical staff skills. The researchers were able to determine that after the five year duration of the intervention in a Guatemalan orphanage, a majority of the trained nursing staff fed children more appropriate amounts, at a slower rate, and improved use of various recommended techniques like properly positioning children (Colodny, Miller, & Faralli, 2015).
Precede-Proceed Example 2
Mbonu, N. C., Van den Borne, B., & De Vries, N. K. (2009). A model for understanding the relationship between stigma and healthcare-seeking behavior among people living with HIV/AIDS in sub-Saharan Africa. African Journal of AIDS Research, 8(2), 201-212.
Mbonu et al adopted the Precede portion of model as an explanatory frame for health care seeking behavior among HIV positive people in sub-Saharan Africa. Researchers were interested in the role of stigma and coping strategies (Mbonu, Van den Borne, & De Vries, 2009). The model identifies the predisposing, reinforcing and enabling factors affecting the outcome of non-utilization of healthcare. It integrates the complex system in which stigma operates and allows stigma to be understood within the social fabric in which it is embedded. The model develops a hypothesis around 3 coping strategies used by the HIV positive population 1) coping with self- resulting in physical, emotional and cognitive problems, 2) coping directed at others, and 3) coping by problem-solving. It describes each of these in detail and assists in understanding healthcare seeking behavior and have implications for HIV programs (Mbonu et al., 2009).
Precede-Proceed Example 3
Ayode, D., McBride, C. M., de Heer, H. D., Watanabe, E., Gebreyesus, T., Tora, A., ... & Davey, G. (2013). A qualitative study exploring barriers related to use of footwear in rural highland Ethiopia: implications for neglected tropical disease control. PLoS Neglected Tropical Diseases, 7(4), 1935-2735.
In a study of shoe-wearing behavior in Ethiopia, Ayode et al examine factors that influence shoe-wearing as it influences prevention of onset or progression of many neglected tropical diseases (Ayode et al., 2013). They used the Precede-Proceed model to understand which social, behavioral, environmental, educational, and ecological issues may impact whether or not children in the study area wear shoes. They identify various influencers, both barriers to and favorable perceptions of shoe wearing that can be used both in future studies and in programs (Ayode et al., 2013). Financial constraints are one of the identified barriers, but the group also found a lack of available shoe types for specific tasks, low risk perception, and fear of stigma from wearing shoes from a free shoe distribution program.
Dynamic Sustainability Framework
Dynamic Sustainability Framework (DSF) was proposed by Chambers and colleagues in 2013 to respond to increasing interest in investigating the sustainability of implemented interventions (Chambers et al., 2013). It embraces change as a central influence on sustainability and anchors its model around seven evidence-based tenants: 1) evidence collected in one narrow context cannot be expected to apply in a vastly different context, so an intervention should not be optimized before implementation; 2) interventions are not static and can be continually improved; 3) evaluation measures need to be relevant to patient outcomes and sensitive to the fit between intervention and context; 4) voltage drop is unavoidable when interventions are rolled out in the real world, meaning over time interventions are not always optimally implemented; 5) fit between setting and intervention is crucial; 6) organizational learning is an essential part of embracing the changes in context and adaptation of intervention; and 7) ongoing stakeholder involvement creates better outcomes (Chambers et al., 2013). It may be most useful when considering interventions in a systematic way and allowing for change in the intervention during the evaluative process. As a fairly new concept there have been few published studies that use this framework.
Two key terms used in discussions of DSF are voltage drop and program drift. Voltage drop means that interventions are expected to be less beneficial in the real world than in the controlled environment of a clinical trial or the lab where they were developed (Chambers et al., 2013). Program drift occurs when deviating from the protocol developed and applied in a controlled environment and yields decreasing intervention benefit in the real-world setting (Chambers et al., 2013).
Traditionally, interventions are created in a controlled environment and then expected to perform at least somewhat worse in real-world practice (Chambers et al., 2013). DSF opens the door to a different approach to implementation that incorporates, “adaptive, contextually sensitive quality improvement (Chambers et al., 2013).” Examples of the use of this framework are not available in the literature at this time.
Practical, Robust Implementation and Sustainability Model (PRISM)
Figure 2: Practical, Robust Implementation
and Sustainability Model (PRISM)
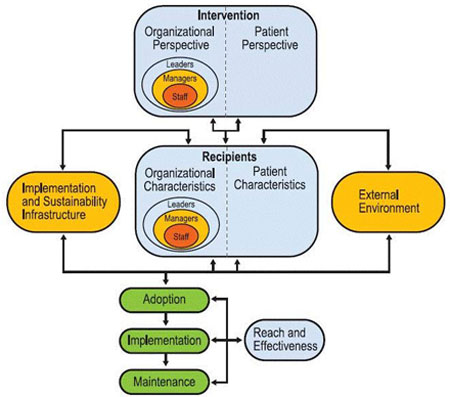
Source: Feldstein & Glasgow, 2008
Full description of
Figure 2: The Practical, Robust Implementation and Sustainability Model (PRISM):
Top intervention box includes organizational (leaders, managers, staff) and patient
perspective. Intervention flows into and out of recipients box, which contains organizational (leaders, managers, staff) and patient characteristics. Recipients affected by implementation and sustainability structure, and external environment, which impact and are affected by the recipients. Below, adoption, implementation, and maintenance flow out of relationships between recipients, implementation and sustainability infrastructure, and external environment; and interact with reach and effectiveness.
Feldstein and Glasgow, outlined the Practical, Robust Implementation Sustainability Model (PRISM) in 2008 in recognition that advances in healthcare research were not always reaching patients (Feldstein & Glasgow, 2008). The authors developed PRISM as a comprehensive model for translating research into practice relying on multiple aspects of other IS models, as well as the quality improvement literature. The model itself expands upon RE-AIM, Precede-Proceed, and the diffusion of innovations theory also discussed in this section (Liles et al., 2015). Elements of the PRISM model include: 1) the program or intervention, 2) external environment, 3) implementation and sustainability infrastructure, and 4) recipients. Relationships between these factors are visible in Feldstein and Glasgow’s model image, reproduced in Figure 2. This model may be most useful in healthcare delivery contexts when there is a principal concern for the sustainability of the intervention for the population of interest within the specific context.
The authors have identified implementation case studies that highlight each of the elements described. They have also identified relevant questions to each of the PRISM domains and have identified the phase of the project where those questions should be addressed. An illustrative example of how to utilize the model is detailed in Figure 2.
The Practical, Robust Implementation and Sustainability Model (PRISM) Example 1
Liles, E. G., Schneider, J. L., Feldstein, A. C., Mosen, D. M., Perrin, N., Rosales, A. G., & Smith, D. H. (2015). Implementation challenges and successes of a population-based colorectal cancer screening program: a qualitative study of stakeholder perspectives. Implementation Science, 10(1), 41.
This study, set in a relatively high-resource context in the US, can provide insight into the application of PRISM to analyze effectiveness of implementation of an intervention in a low resource setting. Liles et al use PRISM to describe the challenges and facilitators of implementing their program for colorectal cancer screening at the system-level. The authors built this implementation study on the back of an earlier clinical trial that evaluated effectiveness of their intervention in the clinic setting. In the clinical trial, the intervention was found to facilitate completion of the screening, which requires fecal samples to be taken at home and returned for testing. The authors wanted to learn more about the implementation process using PRISM. First, the authors adapted the PRISM model, as seen in Figure 2 to their specific study conditions creating a conceptual framework to describe and define the four PRISM components in their setting. They performed guided interviews and conducted qualitative analysis examining implementation challenges. Analysis provided valuable information about what worked and what challenges remain.
The Consolidated Framework for Implementation Research (CFIR)
In 2009 Damschroder et al published the Consolidated Framework for Implementation Research (CFIR), designed to encompass constructs that were included in pre-existing implementation theories to offer a more comprehensive theoretical framework for future research. It describes an overarching typology to promote theory development and verification across multiple contexts about whether and why interventions work (Damschroder et al., 2009). Methods employed in CFIR are both qualitative and quantitative. This model may be most useful in developing a theory around the impact of an intervention, considering why an intervention does or does not work.
The five domains defined by the framework include: 1) the intervention, 2) inner setting, 3) outer settings, 4) individuals involved, and 5) the process for accomplishing the intervention. The intervention is defined as the core characteristics of the planned implementation, without being adapted to a specific context. The inner and outer settings comprise the contexts where the implementation process will occur. These vary depending on the implementation, but the inner setting may include a medical center and outlying clinics; whereas the outer setting includes the political, economic and social contexts. The individuals involved are the agents of change, those who have power and influence to seek, experiment with, evaluate, and improve or design interventions. Lastly, the implementation process describes an active progression where an individual or organization moves toward attaining the outcome of the intervention described. Other constructs described by Damschroder breakdown each of these five domains further into more manageable components for planning and execution (Center for Clinical Management Research, 2014; Damschroder et al., 2009).
Consolidated Framework for Implementation Research (CFIR) Example 1
Sherr, K., Gimbel, S., Rustagi, A., Nduati, R., Cuembelo, F., Farquhar, C., ... & Gloyd, S. (2014). Systems analysis and improvement to optimize PMTCT (SAIA): a cluster randomized trial. Implement Sci, 9(55), 5908-9.
Sherr et al executed a two-arm, longitudinal cluster randomized trial in Cote d’Ivoire, Kenya, and Mozambique one component of which was to evaluate the implementation process using the CFIR. Their intervention, called a five-step, facility-level systems analysis and improvement intervention (SAIA) was designed to improve the prevention of mother-to-child transmission of HIV (PMTCT). It provides tools that are designed to guide program staff decision making at the facility level to identify ways to improve PMTCT.
The study’s primary outcome was the number of women and children pairs who progressed though the PMTCT cascade from screening the mother at the first antenatal visit to screening the infant. The study team integrated qualitative data collection using the CFIR framework to describe intervention characteristics that influenced the intervention’s success. This article lays the groundwork for the protocol. The study is still in process and results are forthcoming.
Consolidated Framework for Implementation Research (CFIR) Example 2
Halek, M., Dichter, M. N., Quasdorf, T., Riesner, C., & Bartholomeyczik, S. (2013). The effects of dementia care mapping on nursing home residents’ quality of life and staff attitudes: design of the quasi-experimental study Leben-QD II. BMC geriatrics, 13(1), 53.
This study examines the person-centered care approach to dementia care mapping (DCM) in Germany to evaluate the intervention for effectiveness in the German nursing home setting in a quasi-experimental design. Authors intend to use findings to inform policy and practice, as well as a formative step in developing a subsequent randomized control trial.
Halek et al use the CFIR framework to study the factors that influence the implementation of DCM in a process analysis. Quantitative data including a staff questionnaire, structural data, and environmental data were analyzed. Qualitative data including interviews with staff were analyzed using the themes and structure of CFIR.
Consolidated Framework for Implementation Research (CFIR) Example 3
Shelley, D., VanDevanter, N., Cleland, C. C., Nguyen, L., & Nguyen, N. (2015). Implementing tobacco use treatment guidelines in community health centers in Vietnam. Implementation Science, 10(1), 142.
Shelley and colleagues are executing a cluster randomized trial to compare two different systems level interventions to treat tobacco use in Vietnam (Shelley, VanDevanter, Cleland, Nguyen, & Nguyen, 2015). They use CFIR as the conceptual framework to examine the factors that facilitate successful implementation. Authors use CFIR at the systems level to organize the study design by intervention characteristics, outer setting, inner setting, and individual characteristics of patients and providers. The study is ongoing and results are forthcoming.
Works Cited
- Ayode, D., McBride, C., de Heer, H., Watanabe, E., Gebreyesus, T., Tora, A., . . . Davey, G. (2013). A qualitative study exploring barriers related to use of footwear in rural highland Ethiopia: Implications for neglected tropical disease control. PLOS Neglected Tropical Diseases, 7(4), 1935-2735.
- Center for Clinical Management Research. (2014). Consolidated Framework for Implementation Research. Retrieved August 12, 2015, from
https://cfirguide.org/
- Center on Knowledge Translation for Disability Rehabilitation Research. (2013, November 20, 2013). Knowledge Translation: Introduction to Models, Strategies, and Measures. Retrieved June 30, 2015, from
http://ktdrr.org/ktlibrary/articles_pubs/ktmodels/index.html#cihr
- Centre for Behaviour Change at University College London. (2015). Resources about behaviour change techniques and theories. Retrieved July 2, 2015, from
http://www.ucl.ac.uk/behaviour-change
- Chambers, D., Glasgow, R., & Stange, K. (2013). The dynamic sustainability framework: Addressing the paradox of sustainment amid ongoing change. Implement Sci, 8(1), 117.
- Colodny, N., Miller, L., & Faralli, M. (2015). The development of a feeding, swallowing and oral care program using the PRECEDE-PROCEED model in an orphanage-hospital in Guatemala. Int J Speech Lang Pathol., 17(2), 1754-9515 (Electronic).
- Damschroder, L., Aron, D., Keith, R., Kirsh, S., Alexander, J., & Lowery, J. (2009). Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implement Sci, 4(1), 50.
- ExpandNet. (2004). ExpandNet: Scaling Up health Innovation. Retrieved August 11, 2015, from
http://expandnet.net
- Feldstein, A. C., & Glasgow, R. E. (2008). A practical, robust implementation and sustainability model (PRISM) for integrating research findings into practice. Jt Comm J Qual Patient Saf, 34(4), 228-243.
- Fogarty International Center. (November 1, 2014). Implementation Science Information and Resources. Retrieved June 30, 2015, from
http://www.fic.nih.gov/researchtopics/pages/implementationscience.aspx
- Glanz, K., Rimer, B., & Viswanath, K. (2008). Health behavior and health education : Theory, research, and practice (4th Ed. ed.). San Francisco, CA: Jossey-Bass.
- Glasgow, R., Vogt, T., & Boles, S. (1999). Evaluating the public health impact of health promotion interventions: the RE-AIM framework. American journal of public health, 89(9), 1322-1327.
- Green, L. (2015). The Precede-Proceed Model of Health Planning and Evaluation. Retrieved June 30, 2015, from http://lgreen.net/precede.htm
- Green, L. W. (1999). Health promotion planning : an educational and ecological approach. In M. W. Kreuter (Ed.), (3rd ed. ed.). Mountain View, CA :: Mayfield Pub. Co.
- Health Information Research Unit at McMaster University. (2015). KT+ Knowledge Translation. Retrieved July 2, 2015, from
http://plus.mcmaster.ca/kt/Default.aspx
- International Initiative for Impact Evaluation. (2015). International Initiative for Impact Evaluation. Retrieved July 22, 2015, from
http://www.3ieimpact.org/
- Kaiser Permanente Cancer Research Network. (2015). Training Institute for Dissemination and Implementation Research in Health. Retrieved June 30, 2015, from http://conferences.thehillgroup.com/OBSSRinstitutes/TIDIRH2015/index.html
- King, D. K., Glasgow, R. E., & Leeman-Castillo, B. (2010). Reaiming RE-AIM: using the model to plan, implement, and evaluate the effects of environmental change approaches to enhancing population health. American journal of public health, 100(11), 2076-2084.
- Liles, E. G., Schneider, J. L., Feldstein, A. C., Mosen, D. M., Perrin, N., Rosales, A. G., & Smith, D. H. (2015). Implementation challenges and successes of a population-based colorectal cancer screening program: a qualitative study of stakeholder perspectives. Implementation Science, 10(1), 41.
- Mbonu, N. C., Van den Borne, B., & De Vries, N. K. (2009). A model for understanding the relationship between stigma and healthcare-seeking behaviour among people living with HIV/AIDS in sub-Saharan Africa. Afr J AIDS Res, 8(2), 201-212. doi: 10.2989/ajar.2009.8.2.8.860
- MEASURE Evaluation. Fundamentals of Implementation Research. Retrieved June 30, 2015, from https://training.measureevaluation.org/certificate-courses/ir
- Moulin, J., Sabater-Hernandez, D., Fernandez-Llimos, F., & Benrimoj, S. (2015). A systematic review of implementation frameworks of innovations in healthcare and resulting generic implementation framework. Health Research Policy and Systems, 13(16).
- National Cancer Institute. (2015a). Implementation Science at a Glance. Retrieved June 30, 2015, from
http://cancercontrol.cancer.gov/IS/glance.html
- National Cancer Institute. (2015b, April 29, 2015). Implementation Science: Integrating Evidence into Research, Practice and Policy. Retrieved June 30, 2015, from http://lgreen.net/precede%20apps/preapps-NEW.htm
- National Implementation Research Network. (2013). Active Implementation Hub. Retrieved August 11 2015, 2015, from
http://implementation.fpg.unc.edu/
- Nilsen, P. (2015). Making sense of implementation theories, models and frameworks. Implement Sci, 10, 53. doi: 10.1186/s13012-015-0242-0
- Research Center on Knowledge Translation for Disability Rehabilitation. (2015, June 2, 2015). Knowledge Translation Library. Retrieved June 30, 2015, from
http://ktdrr.org/ktlibrary/
- Rogers, E. (1995). Diffusion of Innovations 4th Ed. New York, 15-23.
- Shelley, D., VanDevanter, N., Cleland, C. C., Nguyen, L., & Nguyen, N. (2015). Implementing tobacco use treatment guidelines in community health centers in Vietnam. Implementation Science, 10(1), 142.
- Spring, B. (2007). Bridging Research and Practice: Evidence-Based Behavioral-Practice. Retrieved November 12, 2015, from
http://www.ebbp.org/
- Spring, B., Ferguson, M. J., Pender, D., & Starin, A. (2007). Implementation of Evidence-Based Practices. Retrieved November 12, 2015, from http://www.ebbp.org/course_outlines/implementationmoduleoutline.pdf
- Tabak, R. G., Khoong, E., Chambers, D. A., & Brownson, R. C. (2012). Bridging research and practice: models for dissemination and implementation research. American Journal of Preventative Medicine, 43(3), 1873-2607 (Electronic).
- Vickrey, B., Hirtz, D., Waddy, S., Cheng, E., & Johnston, S. (2012). Comparative effectiveness and implementation research: directions for neurology. Ann Neurol, 71(6), 1531-8249.
- World Health Organization. (2014). Implementation Research Toolkit. Retrieved May 5, 2015, from http://www.who.int/tdr/publications/topics/ir-toolkit/en/ (current URL:
https://apps.who.int/iris/handle/10665/110523)
This toolkit is a product of and for the
Learning Collaborative for Implementation Science in Global Brain Disorders, which was initiated and is hosted by the Center for Global Health Studies at the Fogarty International Center, National Institutes of Health (NIH), and was developed in collaboration with members of the Learning Collaborative.
Partners in the Learning Collaborative include the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), the National Institute of Mental Health (NIMH), the National Institute of Neurological Disorders and Stroke (NINDS), the National Institute on Aging (NIA), the Society of Neuroscientists of Africa (SONA), and the International Brain Research Organization (IBRO).
Updated June 21, 2023