Focus on mobile health: Scientists develop app to diagnose, treat leishmaniasis in Colombia
January / February 2020 | Volume 19, Number 1

Photo courtesy of Centro Internacional de Entrenamiento e
Investigaciones Medicas
An mHealth app developed and tested with Fogarty support
helps a health worker evaluate patients with suspected
leishmaniasis lesions in a remote area.
By Susan Scutti
Cutaneous leishmaniasis - caused by bites from infected sandflies - produces skin lesions that leave behind both scars and stigma that last a lifetime. Up to 1.2 million
new cases are diagnosed each year across the 90 countries where the disease exists, including Colombia.
“Leishmaniasis happens where the medical system
isn't," says
Dr. Eliah Aronoff-Spencer, a Fogarty mHealth grantee at the University of California, San Diego (UCSD). He's been working in rural Colombia to bridge the access gap between remote communities and the public health system, using a mobile tool that empowers community health workers to identify new cases of the disease and monitor treatment.
Aronoff-Spencer's team adapted an existing informatics structure to serve as an end-to-end solution for diagnosis and management of the neglected tropical disease, and then ran a pilot study comparing mHealth-assisted care to standard care.
When considering how to design an mHealth solution for use in the city of Tumaco, he realized stakeholder input would be critical to ensuring the tool would be accepted. “We have so much implicit expectation of how these technologies work here in the U.S. and it's not necessarily how they work there," says Aronoff-Spencer. “We had to consider everything from the safety of using cellphones in a FARC-controlled, war-torn area, to how people there use cellphones and what their assumptions are." A firm believer in participatory design, his app developers included the village leader, a variety of community volunteers and the region's professional medical providers, in addition to the U.S. team.
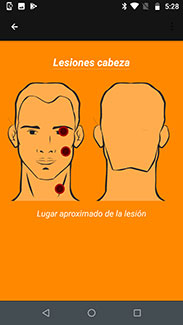
Image courtesy of Dr. Aronoff-
Spencer and his team.
mHealth app for leishmaniasis
The result? A mobile health app built for lower-cost Android phones that can be used by advanced medical practitioners, while also being accessible to community health workers and patients who have lower levels of education. The app allows for patient data and image input, and provides a validated decision-rule to help community health workers assess the possibility of a leishmaniasis diagnosis. Based on decisions made by health workers, the app then refers some patients for laboratory testing and, if a positive diagnosis is the result, the app monitors a patient throughout treatment.
The team recruited 75 patients for a comparison study to see if the mHealth intervention was more effective than standard care. Despite poor access to mobile networks, the app remained completely functional throughout the study period. Results revealed that the app provided clear benefits over standard care, in both treatment adherence and followup.
Aronoff-Spencer is planning further enhancements. “It's our intention to use machine learning and artificial intelligence to combine the pictures of lesions with history and prevalence in the area to come up with predictive models to
automatically diagnose leishmaniasis," he says. Beyond that, the app might one day contribute to Colombia's national registry for the neglected disease, though clear evidence is needed to prove the app is highly accurate, appropriately used and interoperable with Colombia's public health systems.
Among the
project team's achievements was the provision of training to seven community health workers in villages with the highest incidence. So far, they've published
one scientific paper on how to build mHealth tools for neglected tropical diseases and are preparing others to detail the app's performance and clinical outcomes. In particular, Dr. Nancy Gore Saravia, co-principal investigator and scientific director at Centro Internacional de Entrenamiento e Investigaciones Medicas (CIDEIM), part of Colombia’s National System of Science, Technology and Innovation, deserves credit for catalyzing this research effort, said Aronoff-Spencer.
As co-inhabitants of this planet, everyone’s participation is needed to overcome the most challenging diseases, says Aronoff-Spencer: “A research ethic that is more inclusive and promotes the diversity of people and their expertise and opinions in creating solutions will enable you to develop better, more successful, more impactful technology that will help more people.”
It's especially critical to provide active disease surveillance and management in low-resource settings since pathogens are not static, Aronoff-Spencer says. Diseases can move - from markets where animals and humans interact causing new respiratory viruses, from the jungle where Ebola sprung forth, and from the area south of the U.S. border where dengue and zika viruses circulate, he says. “We need to enable people in the communities where diseases are to be first responders and even to carry the torch of research that helps us all."
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.