Focus on mobile health: Mobile tool designed to alleviate late-stage cancer pain
January / February 2020 | Volume 19, Number 1
By Susan Scutti
Witnessing her late-stage cancer patients’ horrific pain in rural Tanzania—and being helpless to control it—prompted oncologist
Dr. Susan Miesfeldt to consider developing an mHealth solution to alleviate suffering where there is no access to care.
It’s an enormous and growing problem. Sub-Saharan Africa currently experiences at least 500,000 cancer deaths each year. Estimates project a doubling of cancer mortality in the region within the next decade. In remote or underserved areas, Miesfeldt says cancer patients have few options for pain relief, beyond seeking assistance from a traditional healer.
There are significant barriers. Often, patients are not diagnosed so they remain unknown to health providers, while many lack the means to travel to and pay for care in a clinic or hospital. Add to that, the only available medicine is oral morphine, which is subject to restricted distribution, plus there's a general lack of awareness of palliative care, says Miesfeldt, an investigator at the
Maine Medical Center.
Why not deploy mobile technology to fill these gaps? Miesfeldt and her team used Fogarty funding to produce and test an app, called the m-Palliative Care Link, that works as a three-way communication system.
“It connects the oncology professionals with patients in their communities and also links in the local health worker. If the palliative care professionals can’t get to the patient, the local health worker can support the assessment of pain and its management of that patient,” says Miesfeldt. Among its virtues, the app allows for the collection of data and the delivery of information by way of a smartphone, tablet or PC, while possessing an intuitive interface that is easy to follow by low-literacy users.
m-Palliative Care Link App
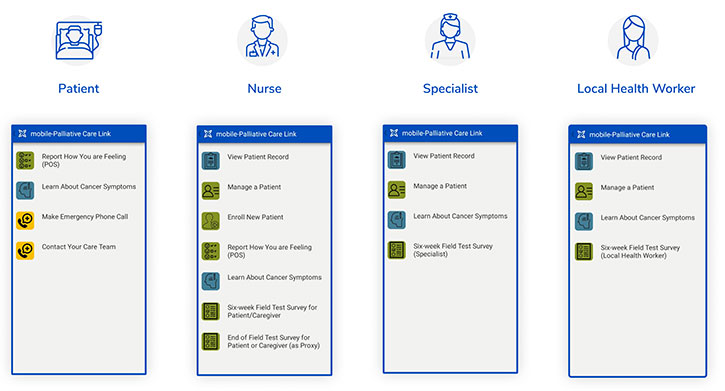
Image courtesy of Dimagi, Inc.
A Fogarty-funded mobile app aims to reduce suffering among cancer patients, especially those living in remote areas without access to care.
Miesfeldt’s two year grant allowed her to design the new app in partnership with Tanzanian local researchers and specialists. Fogarty funding is also supporting field studies, including usability testing by multiple user groups and a
comparison of outcomes among 45 late-stage cancer patients versus a control group receiving the usual care.
Concerns accompanied the creation of her innovative mHealth device. Miesfeldt worried that developing a smartphone app - instead of a cellphone text message system - might be too advanced for Tanzania.
Her tech-savvy team anticipated an increase in uptake of smartphones as the project rolls out, which, indeed, is occurring: Smartphone use has been climbing by almost 20% a year.
“I cannot stress enough the importance of assembling a multidisciplinary team and drawing on the unique expertise of each member so that the tool is both usable and adaptable as technology advances,” says Miesfeldt, who adds her partners “provided tremendous insight” throughout the development process.
It’s also crucial to build community trust to increase understanding of patient and health care workers’ needs in LMICs, says Miesfeldt, who has cultivated relationships in Tanzania since her first visit 10 years ago.
Not only has the project resulted in a tool that might alleviate suffering, it has also provided training and mentoring to local investigators, including Dr. Mamsau Ngoma, a local oncologist, who played a key role in the analysis and reporting of project data. The importance of building research capacity in lower-income nations is not lost on Miesfeldt.
“Currently, a majority of cancer deaths globally take place in countries like Tanzania,” she says, adding that this translates to a need for more research. Still, she emphasized that her team designed their innovative app to be generalizable and scalable to any country, no matter the income level, says Miesfeldt. She herself lives in Maine and can see using the mobile tool to reach remote patients in her state, as well as in other rural areas of the U.S.
More Information
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.
Related Fogarty Programs
Related World Regions / Countries
Related Global Health Research Topics