The paradox of antimicrobial resistance in India
May / June 2022 | Volume 21 Number 3
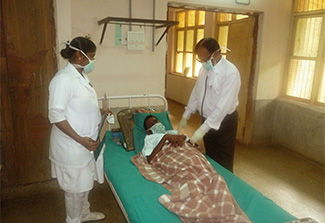 Photo courtesy of Tony Fredrick / CDCIndian medical staff care for a patient with multi-drug resistant tuberculosis. India has one of the highest rates of antimicrobial resistance (AMR) in the world.
Photo courtesy of Tony Fredrick / CDCIndian medical staff care for a patient with multi-drug resistant tuberculosis. India has one of the highest rates of antimicrobial resistance (AMR) in the world.
India, home to one in every six people on the planet, has one of the highest rates of antimicrobial resistance (AMR) in the world. As a Fogarty Global Health Fellow, Dr. Matt Robinson worked in Pune, India, to characterize the burden of antimicrobial resistance among hospitalized patients with fever illnesses. “Fever is the most common reason why people in India seek medical care and we found that almost every patient hospitalized with fever received antibiotics—despite mosquito-borne diseases, which are not treated by antibiotics, being the cause of most of these illnesses,” said Robinson.
There’s a perception that Indian doctors over-prescribe antibiotics, yet that is not entirely true, said Robinson. In resource limited settings, where patients might not be seen by a nurse for 24 hours, options are limited. "So sometimes you provide treatment for the worst possible scenario,” like prescribing antibiotics before identifying the cause of illness.
Other challenges faced by Indian doctors include the many different drivers of AMR. First, there’s limited access to safe water, sanitation and hygiene. Second, many Indians self-medicate without knowing how to use the drugs appropriately. Third, resistant organisms and infections circulate more freely, said Robinson. “Carbapenem-resistant organisms are about 20 times as common in India as they are in the U.S. while about two-thirds of all carbapenem-resistant
Klebsiella and
E. Coli bloodstream infections occur in India.”
The Drug Resistance Index, a measure of efficacy of antibiotic treatments across nations, records generally higher rates of resistance for priority pathogens in LMICs, with India showing the highest rate of all.
“Are more patients in India dying from AMR infections or from lack of access to antibiotics? The answer is lack of access to antibiotics,” said Robinson. “In one place you have this weird paradox, where overall you have insufficient access to antibiotics, yet some patients receive antibiotics inappropriately.”
Multipronged approach needed
The country has reached a “certain tipping point” where antimicrobial resistance is rampant, so Indian doctors prescribe last line antibiotics to everyone and this in turn makes resistance even worse, explained Robinson. “It becomes this horrible spiral where AMR is increasing, so clinicians begin to prescribe ever-broader spectrum antibiotics.”
Perhaps ironically,
India is the world’s top producer of antibiotics, supplying over 40% of the global market, according to a report published by the not-for-profit Stockholm International Water Institute. This, too, contributes to the nation’s AMR problem with high concentrations of antibiotics measured in water bodies surrounding pharmaceutical works and significant contamination of air and soil within manufacturing zones. Along with poor management of pharmaceutical waste, the widespread use of antibiotics in animals and crops also contributes to high AMR rates in India. Human health is affected when antibiotic-resistant bacteria are transmitted between people and animals through contact, food products, and the environment.
Multiple drivers of AMR means solving this problem requires a “multipronged approach,” said Robinson. “The government of India is working very hard to improve infection prevention and control in health care facilities, while making general improvements in sanitation.” Enhanced healthcare systems are also required so patients have access to trained medical professionals and not just the pharmacy counter. Increased access to diagnostics would help doctors become better stewards of antimicrobials. Most importantly, new antibiotics are needed, said Robinson. In the past few years, novel drugs have become available, but they only work against resistance commonly seen in the US. “None of them target the mechanisms of resistance common in India.”
More Information
- Scientific publications
-
Drug Resistance Index, developed by the Center for Disease Dynamics, Economics & Policy
Updated June 15, 2022
To view Adobe PDF files,
download current, free accessible plug-ins from Adobe's website.
Related World Regions / Countries